Sharie Fetzer, the chair of Lipoedema UK, tells Health Europa Quarterly about the charity’s efforts to raise awareness and boost diagnosis of the little-known condition of lipoedema.
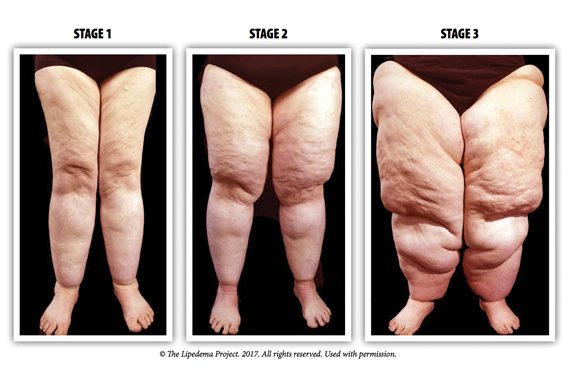
Lipoedema is a chronic condition whereby fat cells abnormally build up in the hips, buttocks, legs and occasionally arms of women (and, far more rarely, men), resulting in often painful pockets of fat that do not go away with exercise or dietary changes. The condition varies in appearance from woman to woman, but every woman with lipoedema suffers from a frustrating lack of awareness among the public and medical community alike.
Lipoedema has been little researched, is rarely taught and is poorly understood; as a result, it is frequently misdiagnosed as obesity or lymphoedema (swelling that occurs due to the lymphatic system not working properly) and only limited treatment options are available.
Lipoedema UK was set up in 2012 by women with lipoedema and St George’s Hospital, London, in order to educate doctors, health practitioners and the public about lipoedema and its symptoms, with a view to improving diagnosis numbers and ensuring that women get the advice and treatment they need to live well with the condition and avoid related complications.
Pan European Networks speaks to the charity’s chair, Sharie Fetzer, about the support available to women with lipoedema, its relationship with obesity, and efforts in the UK to raise awareness and improve understanding.
How much is currently understood about the cause of lipoedema?
The cause of lipoedema is a complete mystery. It’s most likely a combination of hormones and genetic factors, alongside an incident like childbirth, the menopause, or most often the onset of puberty. In the last couple of years more research has been going on to look into it – we are currently working on a genetics project with St George’s Hospital and the Royal Derby Hospital in Nottingham, for instance, which is looking into family trees and lipoedema across generations – but very little is understood at the moment.
How far has awareness of lipoedema increased since the launch of Lipoedema UK in 2012?
There is quite a lot of information on the internet and there are a number of social network groups spreading awareness of the condition, but something we as a charity have focused on specifically is working with the medical community to make sure that their awareness has increased.
Working with patients is an important part of what we do, but what we really want to achieve is to make sure that everyone who completes medical training becomes aware of lipoedema and is able to diagnose it correctly.
We are contacted frequently by patients who are about to undergo treatment for cancer or are having a knee or hip replacement, for example, and want to know how that might affect their lipoedema, or if there’s any information they should give their oncologist or surgeon – because often the people involved in delivering that care have very little knowledge of the condition.
So we do a lot of work with health practitioners because only when awareness improves and diagnosis numbers go up will we get real interest in lipoedema as a condition and start to see proper treatment paths become available to everybody.
How far has that increase in awareness come alongside an increase in diagnosis rates?
Diagnoses are up – we know that thanks to the feedback we get from our members. I’m particularly aware of one case where a woman had been seeking help from her GP for a problem with her legs for 20 years to no avail, and it was only when she joined Lipoedema UK that the GP realised the patient had been right and did have a diagnosable condition – lipoedema.
Since then, her two daughters and her mother have been diagnosed with lipoedema, and she’s discovered that many of her cousins and aunts have it. This led to an invitation to the woman’s GP surgery to make a presentation to the whole practice on lipoedema, so that’s a very obvious example of how the information we’ve provided has really helped someone individually as well as transforming their GP practice.
What is the relationship between lipoedema and obesity, and how far does confusion between the two complicate diagnosis and treatment efforts?
The growing awareness of lipoedema means that some of our medical advisors are being invited to deliver presentations about it at obesity-related conferences and events, which is crucial because obesity and lipoedema are a very dangerous combination: obesity exacerbates lipoedema and makes it harder to treat. However, Lipoedema is not caused by obesity.
At the same time, we need more people to be able to distinguish between the two so that lipoedema can be diagnosed and treated appropriately. Gastric bypass and other surgical weight loss procedures can improve obesity but they are unlikely to improve lipoedema, and it can be very distressing for a patient if they haven’t been prepared for that.
The good news is that bariatric surgeons are now beginning to show more interest in lipoedema and are keeping an eye out for it, and monitoring the long-term success specifically on lipoedema patients. But there is definitely still progress to be made and we specifically want to encourage women who also have obesity to do their best to reduce or control it, as it will make managing their lipoedema much easier in the long run.
What treatment options are available to women with lipoedema and how accessible are they in the UK?
Lipoedema treatments are not very accessible at all. Women usually have to know exactly what it is they want and either find it themselves or put it forward as a suggestion to their GP.
Referral to a lymphoedema clinic is one possibility, and that typically involves conventional treatments such as lymphatic drainage (for pain) and compression (garments particularly), and advice about appropriate exercise and lifestyle choices – as well as support for the many psycho-social issues that are so problematic for many.
Another option is liposuction to reduce the size of lipoedema areas and lessen the associated pain, but this has a number of problems. A certain type of liposuction is available on the NHS if the patient has lymphoedema as well, and a number of women have been successful there, but usually only because they were quite extreme cases.
It’s virtually impossible, however, to get funding for tumescent liposuction on the NHS, and to my knowledge no one who has been diagnosed with just lipoedema has actually gone down that route. This means a growing number of women are forced to fund it themselves and many choose to go abroad where there is more choice and more experienced surgeons.
Tumescent liposuction is certainly a very good choice for women who can afford it and, where suitable, it’s had well-documented success at certain clinics in Germany, the Hanse Klinik in Lubeck, for instance, but it’s not an absolute cure, and patients who do undergo the surgery will still have to do a lot to keep on top of their condition. Younger patients are more likely to have better success rates and a quicker recovery.
What’s also frustrating about the UK is that patients in Germany who have tumescent liposuction receive conventional compression treatments beforehand funded by their government, so in many ways they’re much better prepared for the surgery than women might be here.
What is holding back further progress in treating and understanding lipoedema?
One of the main challenges we face as a charity is actually raising sufficient funds to do the work we need to do. We are a small organisation and we have so few resources because lipoedema is not a condition that necessarily elicits a lot of support or sympathy from other communities. Because lipoedema is so regularly mistaken for obesity, the patient’s lifestyle or genetics are often blamed, as though they just have big legs in the same way that someone else has a big nose or big ears.
Lipoedema is also definitely a women’s condition, and it’s very much to do with appearance and attractiveness, and that has led I think to it being ignored and brushed off – mainly by the male medical community. In that sense, I do think the lack of research and interest reflects a broader feminist issue that needs tapping into.
Lipoedema is also dismissed because it doesn’t seem worth paying attention to in the early stages, but actually, as the condition progresses, it does become very, very difficult to live with. It makes ordinary, everyday activities very hard and can be extremely painful, so it does limit women’s choices and restrict their ability to take part in social situations, and it can have a knock-on effect on their self-esteem and job prospects. It can be particularly damaging to a young girl, for example, who can’t buy the same clothes as her friends, simply because of the size of her legs, Derogatory comments at that age can put girls in a very difficult place and lead to debilitating mental health problems too. Some older women have to give up their careers because they can’t find suitable work clothes or fit into uniforms or when their mobility becomes increasingly difficult.
How does Lipoedema UK benefit from its relationship with the International Lymphoedema Framework (ILF)?
The ILF is a small international community, but it’s made up of quite a powerful group of people, and we’re very proud to be a part of it. The fact that lipoedema is going to be featured prominently for the first time at the ILF 2018 Conference in Rotterdam, the Netherlands, in June is a big step forward; ultimately, whether lipoedema will end up being a lymphoedema condition, I’m not sure because although lipoedema very often does turn into a combination of lymphoedema and lipoedema as it progresses, in the early stages it is a quite different problem. It will be interesting to see how new treatments emerge to deal with those differences – at the moment we are following the path set by lymphoedema specialists, but in the future I can see more options becoming available for people specifically with lipoedema. We’re very proud of our involvement with the ILF, but we would like to see more interest from and interaction with the wider medical community as well, because there are lots of different facets to lipoedema that still need to be explored if we are going to find solutions.
What work does Lipoedema UK do to improve the lives of women with lipoedema and further understanding of the condition?
We have achieved much to be pleased with considering that we’re such a new organisation. Something we’re particularly proud of is the GP e-learning course, which was funded entirely by Lipoedema UK and developed in partnership with the Royal College of General Practitioners.1 That has been a huge success so far in terms of raising credible awareness of the condition and making definitive diagnoses possible in a way they simply weren’t before. Linked to that is Lipoedema UK’s 2014 Big Survey of 250 patients and their experiences of lipoedema, data from which supported the development of the course.2
Lipoedema UK supplies thousands of leaflets for women and healthcare professionals free to UK clinics and therapists, and also offers patient members a GP information pack containing articles and information on resources for GPs who may not have received any training on lipoedema, or even be aware it exists.
In 2017, the UK Best Practice Guidelines for the Management of Lipoedema were published.3 Whilst we didn’t fund these directly, the project was funded in Lipoedema UK’s name and we were instrumental in getting it off the ground. Thanks to these efforts, we now have two really reliable publications that people both in the UK and internationally involved in the care of lipoedema patients can refer to. We are incredibly thrilled that we’ve been able to produce these in such a short space of time.
We have also built up a wonderful group of nurse consultants led by Denise Hardy from Kendal Lymphology Centre and Mary Warrilow and Kris Jones from Lymphcare UK, who have been treating lipoedema patients for quite a while. We also deeply value our relationship with St George’s Hospital and, in particular, our patrons, Professor Peter Mortimer and Dr Kristiana Gordon, who we often ask to vet the information we provide. It’s important to us that we stick to the facts, which is sometimes difficult given there’s so little evidence out there.
In addition, we are working closely with the USA’s Lipedema Foundation, which is very fortunate to have quite substantial funds to donate to various research projects.4 Again, that’s working to raise awareness and improve understanding of lipoedema, with a view to boosting diagnosis rates and making possible the development of new treatments.
At least once a year Lipoedema UK runs events to give patients the opportunity to meet nurse consultants and receive personal advice on compression garments etc., to meet manufacturers of suitable products and hear about the latest developments. At our recent conference in Sheffield we tried to encourage patients to take their care into their own hands and focus on the positive things they could do rather than concentrating on the negative aspects of lipoedema. Since then we’ve received a lot of feedback from patients who have told us that we’ve really helped them to change their attitude and become more positive.
While we would never directly recommend a surgeon, if a patient does want to go down the surgery route, we can make the necessary information available to them and support them in that choice, and we also help them to locate clinics in the UK with the specialist skills to treat them.
One of the key findings of Lipoedema UK’s Big Survey was that most patients took an average of 30 years to obtain a diagnosis. Lipoedema UK believes that our work to promote understanding of lipoedema amongst the wider medical community will lead to a much earlier diagnosis for patients.
An early diagnosis will, in turn, enable patients and healthcare professionals to work together to prevent many associated conditions such as obesity, lymphoedema and psychological problems that can develop in lipoedema patients.
Lipoedema UK firmly believes that our work to raise a greater awareness of how challenging lipoedema can be will stimulate more research to uncover the cause and ultimately find a cure for lipoedema in the not too distant future.
This article will appear in issue four of Health Europa Quarterly, which will be published in February.
























Thank you for the article. I have stage 2 lipedema that also effects my arms. After a lifetime of hating my body and not understanding why starving myself didn’t work, I now have answers. I’m grateful but also more depressed. I am always researching and hoping someone will have an answer for this. Thank you for help shedding light on it.
It’s so great to finally hear that the horrible condition is being looked into. I’ve had swelling of my legs since II was 15, I’m now 68. I’ve been to a clinic last year for lympedema (that’s the first in 53yrs!! ).As I kept on at my doctor as getting worse, took a long time , keeping in about it. And the clinic said I also had Lipoedema, as well as lympedema which I was pleased to find out about, as I had dieted for years and still my legs the same. So at least I now know what I’ve got. For most of my life I thought it was to do with the veins, bad circulation!!!!!
I’ve been having a few tests in Kings to make sure what was going on, as my right leg has now got much worse and is much bigger than the left.!! First doctor I saw knew about lympedema and said would send me after the test were done to see someone,to show me how to massage my legs. Then saw another doctor (lady) and she actually said she didn’t know much about this condition. So I don’t know why I saw her. Anyway I’m waiting now on appointment to find out how to do the massages for the lympedema. But no mention of help with the lipedema!! Oh well you never know maybe at last after 53yrs I’ll get some help. I don’t think they realise how painful it is. And difficult to manage, all my life I’ve had to come in from work and rest my legs so I could get to work following day. I was prescribed directics (water tablets)when I was 15 yrs old and nothing else,just had to get on with it.
Good luck with the research.
Regards jean
I have lipedema and what is wonderful that people are only just now finding out about is that a whole food plant based diet that is low glycemic index, no oils and low fat repairs cell walls in the lymphatic and cardiac systems and can reverse at least partially (for me it was a whole stage) lipedema. My body is now proportional for the first time in my life. They need to study such eating. Dr. Esselstyn’s views on cardiac nutrition work for this as well.
I am 35 and the condition was triggered more after pregnancy. I was a size 2 all my life with the occasion of swollen legs . But my life changed after children as it triggered after the birth of my son. I left the hospital more swollen and gained more weight after giving birth! GO FIGUER!?! This is a very hard disorder to deal with! It affects woman mentally and physically and exercise just makes it worse! I eat healthy! No salt and very little sugar which mostly comes from fruits! NOTHING helps! If u need someone for studies or to operate on for studies I’m available! Please help! This is ruining my self esteem
I am 35 and the condition was triggered more after pregnancy. I was a size 2 all my life with the occasion of swollen legs . But my life changed after children as it triggered after the birth of my son. I left the hospital more swollen and gained more weight after giving birth! GO FIGUER!?! This is a very hard disorder to deal with! It affects woman mentally and physically and exercise just makes it worse! I eat healthy! No salt and very little sugar which mostly comes from fruits! NOTHING helps! If u need someone for studies I’m available!
I am 68 years old, I noticed the onset of lipedema after my children were born, around the age of 30. I have had liposuction and endemologie to no avail. I now have the condition in my arms. I am so happy that there is now more research on the condition and hope one day there will be a cure. My mother had the condition but we don’t know of any one else in the family who suffered with this.
Regards Camille Gorringe.
At last a name for my fat knees and thighs. It is an embarrassment for me and has been for my later years. I am a very active senior citizen always enjoying tennis, walking etc . Having to always cover my knees.
I am aged 68 and have just been told that I have Lipoedema as well as lymphodoema. My arms and legs are awful to look at and they feel so heavy that sometimes I really struggle to lift them. This is a really embarrassing condition as people stare at you and just presume you’re fat. I wear full length compression stockings and they’re like instruments of torture, I also get depressed about my situation. Help !!!!
WOW!! I’m so incredibly blown away by this!.I just stumbled across this article by accident and it explains my legs and what’s actually wrong, as any Doctor I’ve ever had has listed my legs being the way they are as obesity.When I was around 14-15 years old my legs specifically thighs and knees area started becoming very noticeably disproportionate to the rest of my body becoming larger.and now at 36 I’ve had some issues arise with my veins in one leg, but none of which explained the size and look/shape of my legs, both my legs when only one has issues involving the veins.none of the Doctors I’ve seen have been able to explain why both my legs are the way they are.All these years I’ve been made fun of because of my legs I only wear pants even on the hottest days because I don’t want to show my legs….I’ve suffered greatly self esteem wise….I’ve starved myself many times, and went to the gym 7 days a week with no results on my legs, my stomach, arms, and face become really skinny and my bottom half remains the same, I kept a journal of caloric intake/exercise journal for one Doctor who at the end of the months of dieting and practically killing myself gym sessions I had lost weight but my legs didn’t have the results that the rest of my body did and that Doctor basically said I didn’t try hard enough and that I must have been lying about my workouts…reading this was a SERIOUS eye opener, and I’m going to present my doctor with this! But I’m wondering now at almost 37 years old is there ANYTHING I can do for the horrible way my legs look? I absolutely hate them, they’re humiliating to say the least. —Gianna
I hear you all, I really do. It’s with a mix of sadness and relief to know this is the condition. I’ve lived with legs I’ve known to be different since my early teens. A constant stress each day, conscious they are tired, feeling bruised and so much bigger than the rest of me, despite a very healthy diet and exercise. The weird large fatty area on the inside of my knees was something that people noticed and stared at even when I was 12. Just under 30 years on, I am not yet diagnosed, but certain I have this condition – I have an appointment in a few weeks and I will insist my doctor looks into this. I have also had 4 operations for varicose veins, and it makes so much sense as to why I have such terrible veins too. I started doing self manual lymphatic drainage and it is helping a little, my legs are relieved, I’m doing this daily for about 25 minutes and it is exhausting but I think worth it so far.