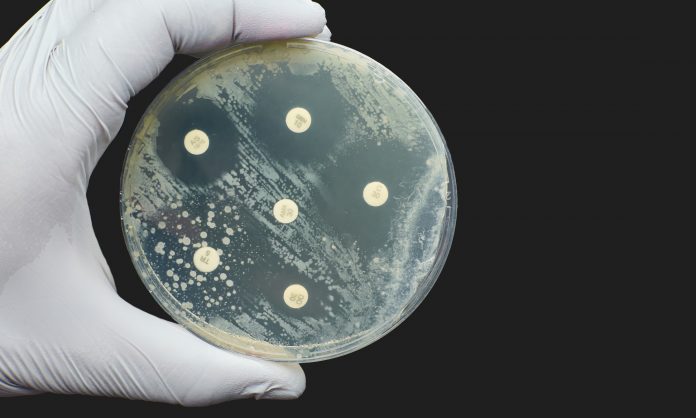
Though often referred to as the silent pandemic, the global consequences of antimicrobial resistance, including resistance to antibiotics, are becoming starkly apparent. Lorna Rothery spoke to Rohit Malpani from the Global Antibiotic Research & Development Partnership to discuss the urgent action needed.
Many will now be familiar with the worrying statistic of ten million deaths from drug-resistant infections by 2050, and the huge threat antimicrobial resistance (AMR) poses to public health and the global economy if interventions are delayed. As global efforts begin to shift from COVID-19 to other pressing pandemics, governments and public health bodies are implementing strategies and initiatives they hope will turn the tide on the worrying outlook for AMR-related deaths. One such organisation dedicated to developing and repurposing antibiotics, and ensuring the most vulnerable people have access, is the Global Antibiotic Research & Development Partnership (GARDP). Lorna Rothery spoke to GARDP’s Policy Advisor, Rohit Malpani about the organisation’s key priority areas for tackling AMR and why we must not overlook the most vulnerable societal groups.
What are GARDP’s key aims and how was your work impacted during the COVID-19 pandemic?
GARDP is a nonprofit that seeks to develop novel antibiotics that address urgent priorities concerning antimicrobial resistance and drug-resistant infections. While we seek to address global needs, we focus especially on the disease burden prevalent in low and middle-income countries and for certain vulnerable populations, such as children.
GARDP is also focused on trying to expand antibiotic access and their sustainable use, including for those that have already been developed. We aim to build a broader revival of the antibiotic field and work with researchers and other stakeholders that have slowly drifted away from the field of antibiotic development.
Our publication, ‘Learning from COVID-19 to tackle antibiotic resistance,’ which we circulated in 2020 sought to examine some of the early consequences of COVID-19 and the lessons learned for resistance to antibiotics.
COVID-19 certainly raised broader awareness of the impacts of infectious diseases around the world and the need to have much greater preparedness. The pandemic also illustrated that not making investments to support pandemic preparedness leads to higher rates of morbidity and mortality, as well as economic consequences.
Resistance to antibiotics can often be conceptualised as a silent pandemic of drug-resistant infections. One distinction is that we know what the potential consequences are and what interventions are required to address resistance to antibiotics, but we still do not have investments in research, development, surveillance, infection prevention and control that are commensurate with the need. COVID-19 could be a reminder that policymakers need to put investments forward and be able to better prepare and respond to resistance to antibiotics.
There were also more tangible operational impacts for GARDP in terms of its ability to conduct some of its operational research and clinical trials that were ongoing and to bring some of our candidate compounds to market.
How can the lessons learned during the COVID-19 pandemic inform long-term response efforts for AMR? Similarly, how can the challenges regarding access to countermeasures during the pandemic be addressed?
There are choices that governments should be making in terms of the amount that they should now invest in the development and access of new countermeasures to address resistance to antibiotics. This includes improving surveillance, diagnostic capacity, infection prevention and control and stewardship. The investments are not yet there that are commensurate with the needs.
In terms of being able to take forward the lessons, it is really a long-term commitment that governments have to make in putting forward the right investments to ensure that the actual crisis that we are now seeing with drug-resistant infections is addressed.
A study from The Lancet emerged earlier this year showing that in 2019, the total number of deaths from resistance to antibiotics reached at least 1.27 million and AMR has played a role in the deaths of at least five million people. We no longer need evidence of the crisis and the need for better preparedness and response, it simply needs to happen.
A second area, certainly for GARDP, concerns how we ensure that there is better cooperation and coherence among all countries related to the response. During the COVID-19 pandemic, even though there were efforts to create mechanisms to ensure greater cooperation among governments, the idea of solidarity faded once a public health crisis emerged which many countries had to tackle at the same time. That speaks to the need to develop better governance mechanisms that can ensure that all countries can respond collectively and equitably to drug-resistant infections.

This requires greater progress in terms of how AMR is managed among governments through mechanisms that have been set up specifically for AMR. This includes the Global Leaders Group for Antimicrobial Resistance, as well as the cooperation among the different UN agencies known as the Quadripartite Joint Secretariat on AMR. We also think that progress requires greater investments in organisations such as GARDP, which was created specifically to address the greatest consequences of drug-resistant infections and is a mechanism for governments to be able to gather their resources – scientific, financial, and human – and address these priority needs.
There are also, of course, responses occurring at the intergovernmental level and the national level; the European Union is especially important. The European Union has always been a leader in the response to resistance to antibiotics and in the aftermath of the COVID-19 pandemic has sought to build a more comprehensive response to AMR, including through the establishment of a new R&D and access authority called HERA. We think this can play an important role in responding to resistance to antibiotics systemically, both within the EU and beyond.
Finally, as it relates to access to COVID-19 countermeasures, there was clear evidence, both during the initial vaccination efforts worldwide and now with the introduction of new treatments, of significant inequity of access, especially between countries, but also within countries. This has really been a lesson in terms of how we try to design mechanisms that do not just rely upon the ability of high-income countries and pharmaceutical companies to look beyond their self-interest but to try to create mechanisms that can ensure we have adequate supply, as well as rules and mechanisms in place to encourage governments to share more equitably and to ensure that vaccines, treatments and tests are directed to where they are required, and where the need is most urgent.
These lessons from the pandemic can apply to AMR. Certainly, we want to ensure that tests and treatments can be provided equitably to all countries and that there is sufficient supply. That is certainly one of the benefits of a non-profit partnership, which can look beyond narrow self-interest, and sustain approaches to the development and access of countermeasures that meet all needs.
How does the One Health concept feed into the collaborative approach to tackling AMR and resistance to antibiotics?
The One Health approach to resistance to antibiotics preceded the COVID-19 pandemic and in some respects, the use of a One Health approach for AMR is now acting as a pathfinder more widely towards prevention and response to infectious diseases.
There is a wider need to recognise that what causes infectious diseases or exacerbates infectious diseases, requires a holistic response that cuts across agriculture and the environment and human health.
A One Health framework has been integrated into how policymakers and professionals seek to respond to antimicrobial resistance, and this can be applied more widely to pandemic preparedness and response. It is certainly one of the reasons why any response to pandemic preparedness whether it is the WHO, or at the national level, would benefit from working with the AMR community. We need to bring together different technical agencies and experts to develop a holistic and comprehensive response.
What are some potential long-term consequences for global public health and the global economy if governments do not act now to support robust interventions?
It is increasingly important to recognise that AMR is no longer a silent pandemic but an urgent crisis. Again, it is underscored by the study that was released earlier this year in The Lancet, which showed that at least 1.27 million people died of drug-resistant infections in 2019. That is also likely to be an underestimate, due to the lack of surveillance in many parts of the world, especially in the African continent. We expect, of course, that the situation will worsen over time as we continue to see a lack of new antibiotics that can respond to these needs, or mechanisms in place to ensure that older first-line antibiotics are available to people, especially in Sub-Saharan Africa and in South Asia.
Given where we are today and the increased resistance that we are seeing to existing antibiotics, that estimate of 10 million drug-resistant-related deaths by 2050 could be far worse. We also know through a study that the World Bank issued a few years ago that the economic consequences of AMR will be significant; it could be as damaging to the global economy as the 2008 financial crisis, with a global increase in healthcare costs between $300 billion to $1 trillion per year. For low and middle-income countries in particular, it would reverse many of the gains that have been made in the last two to three decades.
Although there are significant investments that have to be made in developing new antibiotics and ensuring that they can be used appropriately in health systems around the world, those costs and those investments that have to be made now are substantially less than the human and economic consequences that we could face in the medium to long term.
Can you tell me about the 5 by 2025 initiative and how this is progressing?
The 5 by 25 initiative is progressing well and GARDP is aiming to develop a comprehensive portfolio that will focus on priority disease areas and develop new compounds that address either sexually transmitted infections, such as Gonorrhoea, or serious bacterial infections that are acquired in hospital settings. Importantly, GARDP also seeks to either repurpose existing compounds or ensure that they can be used in pediatric populations which can be especially vulnerable to drug-resistant infections. GARDP is also trying to repurpose existing treatments.
GARDP recently announced a new access partnership and signed an agreement with Shionogi Ltd (and the Clinton Health Access Initiative) to expand access to cefedericol in 135 countries. Our goal is not only to bring new antibiotics to the market and ensure these are used more widely, but that existing antibiotics are accessible to populations that are otherwise neglected by the current system of research and development, and that especially concerns neonates.
Most new antibiotics which have been approved over the last decade tend to be registered and accessible in very few countries, in some cases in less than 10 countries around the world. One of the goals for GARDP is again not only to bring new antibiotics to the market that can be accessible broadly, but when new antibiotics emerge from the efforts of other stakeholders in the public and private sector to be able to work with them to ensure that these are widely accessible and can be used sustainably in different territories, and populations.

Is there anything else you would like to share with our readers?
Serious bacterial infections affect an estimated seven million neonates each year causing over 550,000 deaths. Drug-resistant infections are one of the main drivers of morbidity and mortality among newborns today, especially in low-income countries. As is the case in many different pharmaceutical areas, children and neonates often tend to be the populations that are less focused on, especially because though there is an increased burden from neonatal sepsis and drug-resistant infections, it tends not to be as significant in high-income countries.
Neonates are one of the populations that are most vulnerable to resistance to antibiotics, but neonates tend to be invisible within the wider efforts to build a sustainable pipeline that ensures access to antibiotic products. One of the areas that GARDP is championing, which we really believe is at the heart of the resistance to antibiotics crisis, is both trying to understand the scale of the problem that is facing newborns today and then also seeking to develop solutions. GARDP recently released the results of a study about the morbidity and mortality from neonatal sepsis in several countries and the current response, while also detailing an upcoming clinical trial that seeks to test out the effectiveness of three different treatment combinations. We looked at how different healthcare systems around the world have been responding and how they are prescribing antibiotics to address the needs of neonates. In response to that study, GARDP is now launching a new trial with partners that seeks to test out three different treatment combinations in different countries over the next three to four years to produce better clinical outcomes for neonates that face sepsis in hospital settings.
Rohit Malpani
Policy Advisor
Global Antibiotic Research & Development Partnership
https://gardp.org/
https://www.linkedin.com/company/GARDP
https://twitter.com/GARDP_AMR
https://www.youtube.com/channel/UCW2RQTyCKdON06mEb3wqfKw
This article is from issue 23 of Health Europa Quarterly. Click here to get your free subscription today.
























