Discover how Columbia Care are developing products to meet an unmet clinical need in women suffering from pelvic conditions.
As one of the nation’s most experienced producers of medical cannabis products, Columbia Care is committed to helping patients suffering from a wide range of state permitted qualifying conditions, including pelvic conditions.
It is a fact that female pelvic organs have a very high density of cannabinoid receptors (Brents, 2016). Current knowledge of the endocannabinoid system doesn’t explain the reason for this high number of receptors in the gynaecological urinary tract, but often this system is used to maintain a homeostatic balance in the body. The fact that the vagina has a mucous membrane that can readily absorb medicinal products makes vaginal suppositories uniquely suited to treating conditions affecting the women’s reproductive system, as they target the issue right at its source. It is also obvious that only quality products should be delivered in this manner to avoid irritation and additional inflammation.
The increased public awareness surrounding the use of cannabis for women’s health and the promising research discussed throughout this article put Columbia Care at the forefront of this movement with the debut of their pharmaceutical quality vaginal suppositories. This article summarises the existing scientific evidence regarding cannabis for women’s health concerns, and how these products are already transforming the treatment paradigm for women suffering from these conditions.
Columbia Care is constantly searching for new ways to address conditions associated with women’s health and as a result of these efforts, it has become one of the only medical cannabis companies to develop vaginal suppositories. These are the newest medicinal format addition to their proprietary portfolio of cannabis-based medicines, which already includes tinctures, vaporisation oils and hard-pressed tablets. All formulations are available for women’s health indications (within state guidelines), and for many of these conditions, such as insomnia, one of these traditional formats may be the best option. The vaginal suppositories are an important option for patients who may want rapid delivery of cannabinoids to the pelvic organs.
Cannabis, women’s health and pelvic conditions – current state of research
There is an abundance of anecdotal evidence suggesting that medical cannabis has immense therapeutic potential in women’s health. This section explores the existing scientific evidence for those symptoms and conditions.
Endometriosis
The women’s health condition where inflammation and pain are potentially the most well documented is endometriosis, a condition where tissue that normally lines the inside of the uterus grows in other locations in the body, primarily in the pelvis near the uterus. Women suffering from endometriosis are often in severe pain, particularly during menstruation as this tissue is engorged and also sloughs in response to hormonal cycles.
The long-term consequences of endometriosis are due to inflammation from years of menstrual material that has become trapped inside the pelvis during menstruation, causing irritation and leading to chronic inflammation, strictures and problems with the genitourinary and gastrointestinal tracts. The management of this pain has historically been very challenging, and many treatments for this condition are currently hormone based.
The endocannabinoid system may serve as a target for endometriosis treatments, especially when it comes to pain management. Endocannabinoid receptors interact with these complex pain pathways and are located throughout the body. Two types of cannabinoid receptors are of particular interest: cannabinoid 1 (CB1) and cannabinoid 2 (CB2) receptors. CB1 receptors are highly expressed in the tissues of the uterus and other non-reproductive organs. CB2 receptors are found in multiple tissues, including lung, intestines, pancreas, skin, the uterus and elsewhere (Bouaziz et. al 2017).
Women with endometriosis have lower levels of CB1 receptors in their uterine tissue, and fewer receptors and decreased activation of these receptors may lead to worsening pain. Therefore, increasing the binding to these receptors is of importance in potentially mitigating endometriosis pain (Bouaziz et. al 2017; Dmitreiva et. al 2010), making cannabis a promising treatment option. There are additional pain mechanisms associated with endometriosis and neuropathic pain (nerve pain) that may also add to the discomfort, depending on where exactly the misplaced uterine tissue grows (Bouaziz et. al 2017).
Premenstrual syndrome and premenstrual dysphoric disorder
Patients often report that many symptoms associated with menstrual periods may be alleviated by medical cannabis, and anecdotal reports suggest that cannabinoids are effective in treating menstrual cramps (Robson, 2001). While menstruation is a normal experience among fertile women, many experience premenstrual syndrome (PMS) characterised by feelings of bloating, irritability, tension, breast tenderness and depressed mood. Premenstrual dysphoric disorder (PMDD) encompasses a greater number of symptoms and worsened severity (Slavin et. al 2017).
Current treatment options for PMS and PMDD include lifestyle changes, antidepressants and hormonal interventions. For many women, these treatments are insufficient and may be associated with negative side effects. Given this, medical cannabis may serve as an effective, alternative treatment for these women’s health conditions and may offer fewer negative side effects. Previous findings suggest that cannabis has the ability to mitigate sleep issues, irritability and joint pain, so it may play a helpful role in some of the overlapping symptoms associated with PMS or PMDD.
One recent study of self-reported outcomes demonstrated that women expecting positive results from cannabis treatments achieved relief of PMS or PMDD symptoms. These women used cannabis more often throughout the month, but usage was not associated with cannabis related problems that interfered with interpersonal or professional relationships nor with dependency. (Slavin et. al. 2017). While the exact mechanism for these effects is unknown, the endocannabinoid system may play a role here (Robson, 2001), and one researcher has proposed that the therapeutic effects of cannabis for women experiencing painful periods is a result of anti-inflammatory mechanisms (Russo, 2002).
Insomnia
While not specifically a women’s health issue, the US Department of Health and Human services reports that more women than men suffer from insomnia and that one in four women suffer from symptoms associated with insomnia, such as trouble falling asleep, trouble staying asleep or both. There is strong evidence to suggest that cannabis, specifically products with high amounts of cannabidiol (CBD), can help with these symptoms (Vigil et. al 2018; Babson, Sotille & Morabito, 2017) by reducing symptom severity even more than tetrahydrocannabinol (THC) (Vigil et. al 2018).
A recent review on the topic concluded that, while there is limited research on cannabis and sleep, high doses of CBD can lead to a sedating effect (Babson et. al 2017). One study found that 160 mg/day of CBD increased total sleep time and decreased the number of times that individuals woke up during the night (Carlini & Cunha, 1981). Babson and colleagues are sure to caution that dosage, timing of administration and route of administration all play a role in the efficacy of cannabis products for treating insomnia, demonstrating the importance of products such as Columbia Care’s which are highly consistent, unit-doseable and come in a variety of formats and formulations.
Anxiety
Across the world, the prevalence of anxiety disorders ranges from 2.5 to 7% and varies by country. An estimated 284 million individuals suffered from an anxiety disorder in 2017. Of these, about 63% were female. In all countries, women are more likely to experience anxiety disorders in comparison to male counterparts (Ritchie & Roser, 2018). Scientific data showing that CBD can treat anxiety disorders, including general social anxiety has been published.
More specifically, doses of 300-600 mg of CBD have reduced experimentally induced anxiety in healthy controls and anxiety in patients diagnosed with social anxiety disorder. (Blessing et al., 2015; Hoch et al., 2019). While additional research is needed, this evidence suggests that CBD may be useful in mitigating anxiety in those suffering from anxiety disorders. Anecdotal evidence suggests that patients that receive Columbia Care products experience an improvement in anxiety.
Menopause
In addition to its use for endometriosis, menstrual cramps, and PMS, women with menopause related symptoms are also reporting benefits from cannabis. Insomnia is a known problem in perimenopausal women. A survey-based study conducted in 2016 found that cannabis alleviates certain menopause symptoms, such as sleep problems, irritability, depression and joint pain (Slavin, Farmer & Earleywine, 2016). In addition to these symptoms, some women expected cannabis to relieve hot flashes, vaginal dryness and bladder problems, although evidence for those effects has not been proven (Slavin, Farmer & Earleywine, 2016).
An additional interesting piece of data from this study showed that women’s expectations of how cannabis could help their symptoms did have an effect on the efficacy. This is strong evidence for additional education about the potential benefits of medical cannabis, as women who understood how it might help them were more likely to see a result. Most importantly, researchers concluded that medical cannabis might alleviate menopause symptoms without any negative consequences, suggesting that cannabis is an additional tool for women looking for relief from some of these common symptoms.
Pelvic conditions
Chronic pelvic pain (CPP) is an increasingly reported symptom by women. A recent study found that 100% of patients who used cannabis to address their CPP had a clinically meaningful 5.9-point reduction in pain score, resulting in statistically significant efficacy points (Johns and Lachiewicz, 2019).
An additional study from 2018 supports the use of cannabis to help CPP patients who have not responded to standard treatment options (Nickel, 2018). Experts agree that while it has not been rigorously studied specifically for CPP, medical cannabis is an effective option for treating chronic pain, so it can be assumed that it could be a safe option for CPP patients who have not found success with other treatment options (Hill, 2015).
Sexual health
Finally, there has been much discussion around cannabis and women’s sexual health, with some people claiming that it is an aphrodisiac or that it can improve sexual pleasure. Scientists hypothesise that cannabis acts on these aspects of sexual health through the dopamine system. Dopamine has been shown to drive pro-sexual behaviour, and activation of cannabinoid receptors enhances dopamine (Lynn et. al 2019).
Additionally, cannabis has been shown to lead to an increase in specific hormones, such as oxytocin and testosterone which are known to promote sex drive (Lynn et. al 2019). While sexual arousal and functioning are complicated and difficult to study in a controlled manner, there is data showing that cannabis can play a positive role in promoting sexual health.
One survey of 373 women found that the use of cannabis products before sexual activity increased sex drive and decreased pain (Lynn et. al 2019), reinforcing that women who suffer from low sex drive or experience painful sexual activity might find cannabis a potential solution. In addition, just the vaginal lubrication afforded by cannabis used in a suppository format might provide a more pleasant sexual experience.
Summary
The research referenced here demonstrates that there are several women’s health issues where cannabis can be beneficial. Importantly, many of these indications currently do not have many viable treatment options available except for hormonal therapies, which come with unwanted side effects.
Cannabis could fulfil this unmet need. Columbia Care has developed proprietary, pharmaceutical-quality medical cannabis vaginal suppositories in line with their goal not only to create products that can help women suffering from these disorders but to educate the community about how cannabis can help women in a wide range of health and wellness indications.
Columbia Care vaginal suppositories
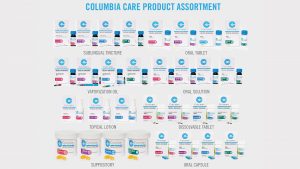
Medicines can be administered by many routes depending on the condition and patient’s needs. Taking these into account, one administration method may be more beneficial than another. This fact holds true for cannabis-based medicines, and because of this, Columbia Care has produced a portfolio of proprietary, precisely formulated, pharmaceutical-quality cannabis-based medicines in many different delivery formats. This portfolio can be divided into four different delivery types:
- Transmucosal administration – This method includes Columbia Care’s tinctures, targeting the oral mucosa under the tongue, and suppositories, targeting both the vaginal and rectal mucosa. These medicines have a relatively short onset of action (15-20 minutes) and an intermediate duration of action (4-6 hours);
- Pulmonary administration – This method includes Columbia Care’s vaporisation oils. These medicines have the quickest onset of action of any of Columbia Care’s formulated products (2-3 minutes), but they also the shortest duration of action (2-3 hours);
- Transdermal administration – This method includes Columbia Care’s topical lotions. These products may have an intermediate time to action, not as fast as mucosal or pulmonary, but faster than oral which requires digestion. This route of administration is likely to be the most variable due to differences in absorption;
- Oral administration – This method includes Columbia Care’s capsules, dissolvable tablets and hard-pressed tablets. These medicines have the longest onsets of action of any of Columbia Care’s formulated products (1.5-2 hours), but they also have the longest duration of action (6-10 hours).
Each of the above formats is also produced in multiple different formulations, including:
- TheraCeed™ – Columbia Care’s high-THC: low-CBD medicines;
- EleCeed™ – Columbia Care’s equal THC: CBD medicine;
- ClaraCeed™ – Columbia Care’s low-THC: high-CBD medicines; and
- ClaraCeed Ultra™ – Columbia Care’s low-THC: ultra high-CBD medicines.
For certain women’s health indications, Columbia Care’s vaginal suppositories can be a welcome relief for many women. Due to their transmucosal administration and the abundance of endocannabinoid receptors in the female reproductive tract, suppositories have the potential to provide significant therapeutic benefit. This delivery format enables the full spectrum of precisely dosed cannabinoids to access these natural endocannabinoid receptors quickly and provide fast, local relief, while also limiting systemic concerns.
As one of the largest medical cannabis operators in the United States, Columbia Care has treated a broad array of women with many different qualifying conditions and finds similar results to those described above. The trained pharmacists at their dispensaries in New York have worked with many women with conditions such as menstrual cramps, difficulty sleeping, painful sex and endometriosis to choose the perfect format and formulation for relief with their proprietary medical cannabis suppositories.
For one Columbia Care patient, vaginal suppositories meant the difference between a potential hysterectomy and a comfortable, pain free life.
“I have endometriosis and multiple sclerosis. Sex was also very painful for me. For my endometriosis when I have severe cramps, I use Columbia Care’s vaginal suppository. Within one hour, I feel amazing and I can go eight hours without pain. It relaxes me for hours and also makes sex less painful. Before using them, my life was very complicated. I have already had one surgery due to my endometriosis and the next step would have been an early hysterectomy. But thanks to these suppositories, I don’t have to go down that route. These medicines relax my body and muscles and make my life more relaxed and comfortable. These suppositories have worked very well for me.” – Ashely
For another patient, their suppositories provide a breast cancer survivor with much-needed pain-free nights of sleep.
“I used to live in pain 24 hours per day. Sleeping was always an issue between my severe chronic pain, my PTSD and my recovery from breast cancer. These suppositories have become a part of my nightly routine and without them, I can’t sleep as well. They are like my security blanket. They also definitely help with my menstrual cramps before my period. My life is greatly improved after using these suppositories.”– Miranda
The Entourage effect
For many of the women’s health indications described in the studies above, the medicinal benefits were achieved with full spectrum cannabis products that include CBD, THC and the numerous additional phytochemicals inherent in the plant. Research shows that the therapeutic benefits of the cannabis plant are enhanced when all the ingredients are used.
The different reported benefits with the whole plant extract are known as the “entourage effect.” For example, CBD in full spectrum is believed to balance out the psychoactive activities of THC, while THC is exerting analgesic properties (Russo & Guy, 2006), making THC less potent in its psychoactive effects. It is important to distinguish data using pure CBD products from full spectrum products that can have an ‘entourage effect.’
Part of the entourage effect mentioned above is due to a class of plant chemicals known as terpenes, which are found in cannabis and other related plants, imparting much of their odour, and may also work in a coordinated manner with cannabinoids. Products that include cannabinoids and terpenes may prove more effective at alleviating pain versus the use of a single agent such as pure CBD (Trevaskis et al, 2009).
Additional information about the role of each Phyto cannabinoid on the endocannabinoid system and their subsequent medicinal benefits would take rigourous scientific study. Many patients and consumers may benefit from medicines that include a full spectrum of therapeutic compounds rather than a single cannabinoid alone, while others may benefit from a single compound. Further evidence-based research is required to match the correct medicine to each condition on a personalised basis to ensure the best clinical outcome.
As a result of this current research and first-hand experience with tens of thousands of patients, Columbia Care ensures that their entire portfolio of formulated, pharmaceutical-quality medicines is comprised of full spectrum products, including their suppositories. They precisely control the concentrations of the top 12 cannabinoids in each of these medicines, and ensure the terpenes and flavonoids are included to provide their patients with the maximum possible benefit.
Columbia Care is leading the way with its focus on women’s health
Columbia Care, with its distinctive and enduring commitment to furthering scientific research and product innovation in the medical cannabis industry, aims to transform the way that the wellness community addresses women’s health issues. Columbia Care’s proprietary vaginal suppositories in TheraCeed, EleCeed, ClaraCeed and ClaraCeed Ultra doses are the first of their kind, marking an important turning point for women seeking respite from their unmet medical needs, which includes debilitating pain.
As can be seen by the testimonies, patients are already experiencing profound therapeutic benefit from their suppositories. As the research into cannabis and women’s health continues to expand, Columbia Care is perfectly positioned to provide the most reliable and consistently dosed products to women who are looking to transform their lives.
References
- Brents LK. Marijuana, the Endocannabinoid System and the Female Reproductive System. Yale J Biol Med. 2016;89(2):175–191. Published 2016 Jun 27
- Bouaziz J, Alexandra B, Seidman D, Soriano D. (2017). “The Clinical Significant of Endocannabinoids in Endometriois Pain Management.” Cannabis and Cannabinoid Research; 2(1): 72-80.
- Dmitreiva N, Nagabukuro H, Resuehr D, Zhang G, McAllister S, McGinty K, Mackie K, Berkley K. (2010). “Endocannabinoid involvement in endometriosis.” Pain; 151(3): 703-710.
- Slavin M, Barach E, Farmer S, Luba R, Earleywine M. (2017). “Cannabis and symptoms of PMD and PMDD.” Addiction Research & Theory; 1-7.
- Robson P. (2001). “Therapeutic aspects of cannabis and cannabinoids.” British Journal of Psychiatry; 178: 107-115.
- Russo E. (2002). “Cannabis Treatments in Obstetrics and Gynecology: A Historical Review.” Journal of Cannabis Therapeutics; 2(3-4): 5-35.
- Vigil, J.M.; Stith, S.S.; Diviant, J.P.; Brockelman, F.; Keeling, K.; Hall, B. Effectiveness of Raw, Natural Medical Cannabis Flower for Treating Insomnia under Naturalistic Conditions. Medicines 2018, 5, 75.
- Babson, K.A., Sottile, J. & Morabito, D. Curr Psychiatry Rep (2017) 19: 23. https://doi.org/10.1007/s11920-017-0775-9
- Carlini, E. A. and Cunha, J. M. (1981), Hypnotic and Antiepileptic Effects of Cannabidiol. The Journal of Clinical Pharmacology, 21: 417S-427S. doi:10.1002/j.1552-4604.1981.tb02622.x
- Ritchie H. & Roser M. (2018). “Mental Health.” Our World in Data. https://ourworldindata.org/mental-health
- Blessing, E. M., Steenkamp, M. M., Manzanares, J., & Marmar, C. R. (2015). Cannabidiol as a Potential Treatment for Anxiety Disorders. Neurotherapeutics, 12(4), 825–836.
- Hoch, E., Niemann, D., von Keller, R., Schneider, M., Friemel, C. M., Preuss, U. W., … Pogarell, O. (2019). How effective and safe is medical cannabis as a treatment of mental disorders? A systematic review. European Archives of Psychiatry and Clinical Neuroscience, 269(1), 87–105.
- Melissa N. Slavin, Stacey Farmer & Mitch Earleywine (2016): Expectancy mediated effects of marijuana on menopause symptoms, Addiction Research & Theory, DOI: 10.3109/16066359.2016.1139701
- Hill, K. P. (2015). Medical Marijuana for Treatment of Chronic Pain and Other Medical and Psychiatric Problems. JAMA, 313(24), 2474.doi:10.1001/jama.2015.6199
- Nickel J. C. (2018). Medical marijuana for urologic chronic pelvic pain. Canadian Urological Association journal = Journal de l’Association des urologues du Canada, 12(6 Suppl 3), S181–S183. doi:10.5489/cuaj.5331
- Becky K. Lynn, Julia D. López, Collin Miller, Judy Thompson, E. Cristian Campian. (2019). The Relationship between Marijuana Use Prior to Sex and Sexual Function in Women. Sexual Medicine. 2019. (1-6). https://doi.org/10.1016/j.esxm.2019.01.003.
Columbia Care, Inc.
info@col-care.com
https://www.col-care.com/
Please note, this article will appear in issue 10 of Health Europa Quarterly, which will be available to read in July 2019.