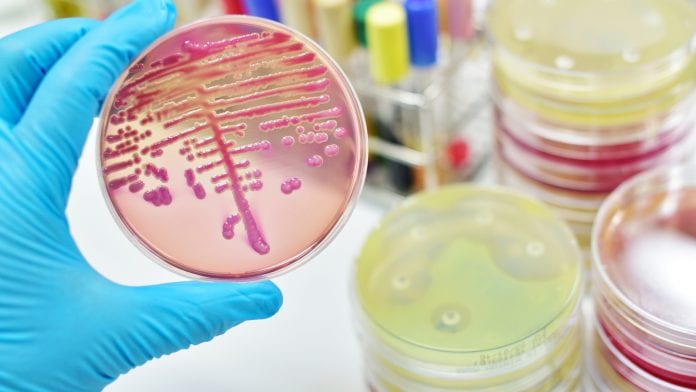
Arlene Brailey, Patient Support Officer at Antibiotic Research UK, discusses the burden of antimicrobial resistance, COVID-19 and the need for targeted research.
Arlene Brailey, interview by Rosemary Lobley
A new report of case studies published in November 2020 has given a platform to people living with drug-resistant infections, people who have survived these infections, and the clinicians who treat them. The Antimicrobial Resistance (AMR) Voices report provides a first-hand look at how the real-life experience and challenges of AMR collide with the realities of COVID-19. Arlene Brailey, Patient Support Officer at Antibiotic Research UK, which contributed to the report, tells Health Europa about the burden of antimicrobial resistance and the need for targeted research.
What are the primary goals of Antibiotic Research UK?
We are the only charity in the UK – for a while we were the only charity in the world – dedicated to fighting the growing global problem of drug-resistant infection. Initially, our goal was to find new treatments which could effectively replace antibiotics: that is still the main goal of the charity, but we now also have a role in education and raising awareness. The charity has also launched the UK’s first patient support service for drug-resistant infections, which came out of the awareness of patients and their families who were struggling with these infections and had nowhere to find information or support, which led to them feeling very isolated and alone.
We offer one-to-one support, as well as access to support groups; we provide people with up-to-date, trustworthy information on antimicrobial resistance. I think the most important thing we do is listen to people and give them encouragement at a time when they are typically feeling very low: we provide a network to discuss the kind of issues that patients are wrestling with; most of all, we help to reduce that sense of isolation that a lot of sufferers feel.
What were the key messages drawn from the AMR Voices project?
The crucial aspect of the project is that we are now hearing the human side of antibiotic resistance through all these case studies, whereas until now, most of the discussion was theoretical. This report highlighted that this is real – it’s not a problem of the future, it is happening to real people right now. The clinicians interviewed for the report talked about how devastating it is to have to tell a patient that their antibiotic treatment isn’t working; that was shocking, because the general public would never expect their doctor to say that, so I think that is a bit of a wake-up call.
The problem can only be solved with a holistic, societal approach; there is not a single solution. Decision-makers, the pharmaceutical industry, the voluntary sector, healthcare workers, and the public all have a part to play in solving this very complex problem. The other thing that the report made clear was that, amidst the COVID-19 pandemic, there was both surprise and frustration on the part of sufferers that the AMR issue had not actually been highlighted more.
Has AMR been overlooked in the drive to address the COVID-19 pandemic? Could increased research and funding help to offset a secondary crisis in drug-resistant infection?
COVID-19 has been such a big, perplexing issue for the general public that a lot of the detail has been passed over. When people die with COVID-19 it can sometimes be the result of a secondary bacterial infection, and I am not sure if the general public is particularly aware of that. That may be one of the things that we need to get much better at: when it comes to certification of death, we need to be more clear if a drug resistant infection has led to that death.
I think the pharmaceutical industry is understanding of the issue, and keen to be involved, but we need to do something much bigger and broader to increase both the funding and the will to do something about this now. AMR Voices found that there is increasing awareness among the public of drug resistant infections, but they feel quite powerless – they don’t know how to make a difference. Increased funding and research would be so welcome, but in addition to that, we need to harness the learning and collaborative efforts which have produced all these COVID-19 practices, treatments and vaccines. If we could harness that in the fight against AMR, I think we would really make huge progress very fast.
What are the primary challenges currently facing the management and treatment of drug-resistant infections? Has the COVID-19 pandemic made things more difficult?
Drug-resistant infections can be treated with a drastically reduced range of antibiotics; and some patients who are seriously ill reach a stage where no orally administered antibiotics will work: their infection flares up, they end up hospitalised and are put on intravenous antibiotics, but the concern is that there will come a point that those antibiotics will also no longer work. We want to develop new combinations which could overcome antibiotic resistance – and perhaps even non-antibiotic treatments, with all the technologies and developments that we are seeing.
Treating antimicrobial resistance is complex, difficult and tedious; and there are still doctors, nurses and pharmacists who maybe don’t understand the issue deeply enough because they didn’t take it seriously enough. We still have issues with overprescribing of antibiotics, which are sometimes prescribed prophylactically, ‘just in case’. We still have some education to do. We need drug resistance to take a higher priority in both medical and healthcare education, so that our professionals know exactly what they’re dealing with and the role that we play. Another issue with managing drug-resistant infections is that the language around it can often confuse the public: the term AMR may sound very meaningful to a health professional, but the person on the street doesn’t understand it.
COVID-19 has shown us all what a pandemic can look like: it’s made us all aware of the huge upset to our lives and the heartache that it can cause if someone close to us becomes very ill or dies; and it has put health much higher on the global agenda, so that must be a help in the fight against AMR. My hope now is that the world will seize this initiative and help us not slide into the potential second pandemic of drug-resistant infections, but this is also a really difficult message to convey to the public right now. COVID-19 has caused a lot of weariness and both mental and physical overload; and people do not necessarily want to hear about the next impending disaster, so although the time is right, we need to be quite thoughtful and careful about how we highlight the next big problem, and we need to try and harness public engagement both during this pandemic and – maybe more importantly – afterwards.
How can public policy be updated to alleviate the burden of AMR and reduce the number of associated deaths?
We need to find a way of developing new antibiotics: there are very few in the pipeline, and a lot of that has to do with the way in which the development of new medicines is funded. Traditionally, the pharmaceutical industry would develop new programmes of drug research and development and when a new drug comes to market, the profits from its sale cover the development costs. That does not work for antibiotics, because when a new antibiotic is develop it will be used very sparingly on infections for which nothing else works; and even when it is used it will only be for a few days, so the classic financial model of drug development doesn’t work for antibiotics. Therefore, governments need to incentivise the pharmaceutical industry to develop new antibiotics in a different way.
The UK government has said that the voluntary sector is in a really good place to educate and support the general public and people who are suffering, but much more resources are needed to better inform people about antimicrobial resistance; and to help people in the way that our patient support services has done, but on a much grander scale – we have a real issue here. People trust charities to provide trustworthy information, to be upfront and honest, and to use evidence-based information; so I think government should work in partnership with charities to reach out with clear messaging and support for those who are suffering. Perhaps policymakers can take what has been learned from the COVID-19 pandemic to increase understanding and awareness in the public. For example, in the same way that we now all fully understand the need for hand hygiene to prevent the spread of infection, we could build on that knowledge and widen that understanding to include the challenges of bacterial infection and what we must do to prevent this next pandemic from occurring.
Arlene Brailey
Patient Support Officer
Antibiotic Research UK
www.antibioticresearch.org.uk
This article is from issue 16 of Health Europa. Click here to get your free subscription today
























