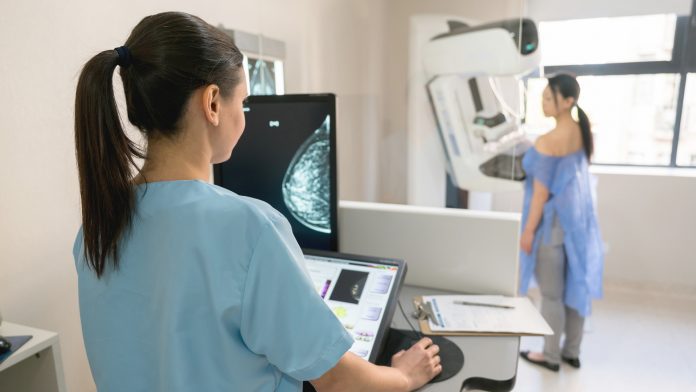
Evidence from a Queen Mary University of London study has revealed that the benefits of the NHS Breast Screening Programme outweigh the small risk of overdiagnosing the condition.
The NHS Breast Screening Programme has a profound effect on combatting breast cancer in the UK, accounting for 31% of all new cancer diagnoses in women yearly. Despite cases increasing by 4% in the last 10 years, deaths caused by breast cancer are declining.
Although screening for the disease is saving lives, the risk of overdiagnosis results in some women not wanting to participate in the screening. Researchers from the Queen Mary University of London have now eased these worries, finding that the risk of overdiagnosis is relatively small compared to the benefits of early identification of breast cancer.
The NHS Breast Screening Programme
The NHS Breast Screening Programme invites females aged between 50 and 70 who are registered with a GP for a breast cancer screening every three years. Screening consists of using x-rays known as mammograms to assess breasts for signs of cancer, although concerns remain about the potential harms of screening, such as overdiagnosis.
Overdiagnosis is not when a test identifies something abnormal that turns out not to be cancer, known as a false-positive, but when a real cancer is diagnosed that would have grown so slowly that it would never have caused any symptoms. Previous estimates on overdiagnosis rates ranged from less than 5% of screen-detected cancers to more than 30%.
How prevalent is an overdiagnosis?
It is essential that women can be confident in overdiagnosis rates to make informed decisions about attending the NHS Breast Screening Programme. To quantify this, the researchers examined 57,493 breast cancer cases diagnosed between 2010 and 2011, matching these with 105,653 controls.
The team estimated the effect of breast cancer screening on breast cancer risk and combined the results with national incidence data to determine the absolute rates of overdiagnosis.
This was calculated as the cumulative excess of cancers diagnosed in women aged 50 to 77 who attended three-yearly screening when aged 50 to 70. The researchers then compared these results with women who did not attend breast cancer screening.
The results showed that the estimated number of cases overdiagnosed in women attending all screens in the NHS Breast Screening Programme was under three per 1000, meaning an estimated 3.7% of screen-detected cancers were overdiagnosed.
This is significantly lower than previously estimated, and the team noted that, at worst, the NHS Breast Screening Programme is associated with a modest overdiagnosis of the disease.
Stephen Duffy, Professor of Cancer Screening, Queen Mary University of London and joint lead investigator, said: “These results provide some reassurance that participation in the NHS Breast Screening Programme confers only a low risk of an overdiagnosed breast cancer. Along with the results of our previous study of the effect of screening on breast cancer mortality, this indicates that the benefit of screening in preventing deaths from breast cancer outweighs the small risk of overdiagnosis.”
Peter Sasieni, Academic Director of the Clinical Trials Unit and Professor of Cancer Prevention at King’s College London, and joint lead investigator, concluded: “Overdiagnosis is quite a complex issue. Had we stopped following women at age 70, nearly 1% of screened women would seemingly have been over-diagnosed, but by waiting another seven years, more never-screened women will be diagnosed with breast cancer, and three-quarters of the excess cancers turn out to have been diagnosed early rather than over-diagnosed. What this means is that most previous studies have overestimated the harms of participating in breast cancer screening up to the age of 70.”






















