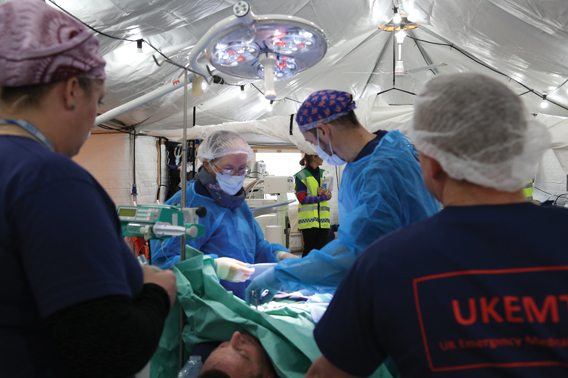
Professor Anthony Redmond OBE, the former chief executive and now chair of the Board of Trustees of UK-Med, considers the challenges involved in delivering emergency medicine in the wake of an overseas disaster.
In the aftermath of a large and sudden-onset disaster or outbreak, the rapid deployment of trained medical staff is crucial in order to save lives and maintain the health of the affected population(s). One organisation working to achieve this is UK-Med, which was established as a charity in 1995 in response to the siege of Sarajevo and has since deployed emergency medical teams (EMT) to such places as China, following the Sichuan earthquake of 2008, and the Philippines, in the wake of Typhoon Haiyan in 2013.
UK-Med recruits healthcare workers interested in disaster relief to its own Community of Practice as well as the government-funded UKEMT programme, which operates at the forefront of the United Kingdom’s response to overseas crises.
In 2014, when the World Health Organization (WHO) declared Ebola a ‘public health emergency of international concern’, UK-Med was instrumental in UK efforts to control the epidemic, enlisting volunteers to work at treatment centres in Sierra Leone and readying vital standby teams for deployment if needed.
UK-Med also works alongside healthcare staff in disaster-prone countries to improve their medical and surgical skills and knowledge, and enhance their own ability to respond to crises.
At its heart is a commitment to combining altruism and humanitarian principles with careful preparation, rigorous training, and the highest standards of healthcare.
Here, Pan European Networks speaks to Professor Anthony Redmond OBE, the former chief executive and now chair of the Board of Trustees of UK-Med, to find out more about the charity’s work to normalise the delivery of emergency care abroad and some of the challenges involved in doing so.
What ethical challenges do medical teams have to consider when delivering emergency care in response to a disaster in another country?
What we try to do is provide a standard of care anywhere in the world that we would expect to receive in our home country. The challenge therefore lies in mass casualty management, or the presentation of a lot of people with serious conditions at the one time. In order to maintain a certain standard of care to the population, we may have to alter the level of care that we give to an individual. That is the essence of triage, and it may mean that we can’t give everyone a complex operation, because if we did we wouldn’t get through all the patients that are presenting to us. We have to prioritise the immediately lifesaving surgery and ask people to wait for further surgery in order for us to get through everybody.
How far do issues such as informed consent and a lack of medical records complicate the delivery of emergency care?
One of the things we have campaigned against is people thinking that, in a large-scale disaster in a more vulnerable country, informed consent is not required, medical records are not required, and identifying yourself to a patient is not required. They are all essential.
If you cannot get informed consent, because the person is too ill, then you would follow the same procedure as you would if someone were to present to an emergency department in this country: if their relatives are with them, you would get the consent of a relative, and you would get it in their own language, meaning you would need to have interpreters with you. If a person presents entirely by themselves and they cannot give consent, because their condition makes them unable to, then you would have to consult with colleagues – as you would in the UK. We have a process whereby ethical decisions like that can be made very quickly.
Likewise, if someone just comes into an emergency department off the street, even if they’ve been treated in that hospital before, you might not be able to access their medical records right away, in which case you would take a medical history and try to gather as much information about them as possible. It’s exactly the same process in a disaster.
We have a great deal of experience in responding to major incidents and dealing with mass casualties, so the process of compiling a medical record and acquiring informed consent are things you should already be familiar with if you’re in this line of work.
Something we’ve been very keen to stress is that delivering emergency care in another country, in the wake of a disaster, is still delivering emergency care, and you should do it just as you would here in the UK. It’s only the environment in which you’re working that’s abnormal; everything else is the same – so you still have to be properly trained, you have to be fully registered, and you have to have certain competences. I think the appreciation of that has improved a lot in recent years.
To what extent do emergency response efforts focus on the prevention of long-term disability in addition to lives saved?
The short answer is not enough. It’s important to understand that while the immediate emergency response is important, it has to feed into a longer term follow-up programme.
We have made the rehabilitation of patients an integral part of our emergency response. To this end we have partnered with Handicap International, an international rehabilitation organisation, and we now have a rehabilitation specialist in our forward team who is there in the operating theatre with us advising on and identifying what the immediate needs will be.
To give a concrete example: when we deployed to Gaza in 2014, the immediate surgical response required turned out to be very limited, but afterwards we joined with experts from Handicap International to carry out a six-month community rehabilitation programme for victims of the conflict.
To do that, it’s important to liaise with the local healthcare services and the ministry of health from the point of your arrival – your patients are still part of the local and national healthcare system, and you’ll need to understand where they will be discharged to and what will be required to support them once they have been discharged. That’s where our partnership with Handicap International is crucial.
Are there any particular challenges involved in working within foreign healthcare services?
Potentially, but in practice I’ve found it more straightforward than you might imagine. The important thing is to make sure that when you respond to a sudden-onset disaster or outbreak you are authorised to practice in that country and you have actually been invited by that country’s ministry of health. Because they’ll know what they want you to do, and that way you can fit into the system. The problems begin when people haven’t been invited and just arrive in a country, only for the host government to have no idea who they are or what capabilities and resources they have.
For this reason, we very much support the WHO Emergency Medical Teams (EMT) Initiative, a system whereby anyone interested in doing this work can register with the WHO and then be classified according to their capacity and resources. Type 1 teams provide outpatient services, type 2 deliver inpatient services, including surgery, and type 3 are a full field hospital. The WHO will inspect what you are offering and provide advice on the kind of personnel mix, drugs and equipment you’ll need, and so on, and once you’re registered, should a disaster occur, the WHO and the host government can compare what’s needed with your offering and, if a match, allocate you a place to work. This can be managed online now via the Virtual On-site Operations Co-ordination Centre.
It’s all about preparing and working with the international organisations before an event – not once a disaster has occurred, but now.
The 2010 Haiti earthquake marked something of a turning point in the international community’s response to humanitarian crises. What in particular inspired this?
Something to have come out of Haiti in 2010 was a concern about inappropriate responses. It’s an unfortunate irony that the most vulnerable countries, and therefore the ones who would most benefit from international assistance, are often the least capable of keeping out the help they don’t want.
The December after Haiti, the WHO and the Pan American Health Organization held a meeting in Cuba, out of which came the Foreign Medical Teams Working Group, or the EMT Initiative as it is now known. That set about recognising the need for standards and verification, and emphasised that people should only work within the competences for which they are trained and recognised in their own country. In other words, if you’re a GP in the UK, you can’t go out and perform surgery in somebody else’s country. The WHO now has an office of full-time staff working on this initiative.
UK-Med played an important part in the response to the Ebola outbreak in Sierra Leone. How much of a role is there for emergency medical teams in outbreak response as well as trauma and surgery?
There is a definite potential and need for healthcare workers to go out and support outbreaks, too, and I think the response to Ebola demonstrated that, but medical teams need to be properly trained to do so. International public health agencies are working very closely with one another to that end, and the UK now has a Public Health Rapid Support Team which works alongside the WHO and the Global Outbreak Alert and Response Network (GOARN) to effectively respond to outbreaks.
What are UK-Med’s priorities looking to the rest of 2018?
What we want to do is help other countries build the same sort of mechanism that we have, i.e. a register and a training programme. We do that by supporting the WHO in its activities, and, as a specific example, we are working with Uganda on a number of initiatives to increase the capacity of its emergency medical teams by strengthening its emergency departments and establishing a pre-hospital care system.
One of the first modern outbreaks of Ebola was in Uganda, so the country already actually has a great deal of expertise in managing an outbreak and could very well have a national emergency medical team in that vein. That’s another thing we’re looking at.
I personally do a lot of work in China, which has some vulnerabilities in terms of its response to emergencies in more rural areas, and so we are working with the Chinese to build up their EMT training programme, as well.
We have about 2,500 volunteers on the register, and one of the challenges we face is actually giving all of them an opportunity to go out and do this work. Something we are looking to our new chief executive, David Wightwick, to do is to expand our work with NGOs like Handicap International so that everyone on the register can be of more benefit to more people.
Professor Anthony Redmond OBE
Chair, Board of Trustees
UK-Med
Tweet @UKMed_NGO
This article will appear in issue four of Pan European Networks: Health, which will be published in February, 2018.























