Inflammacheck offers rapid point-of-care testing of the lungs, supporting healthcare professionals to rapidly identify active lung inflammation
Lung diseases such as asthma, chronic obstructive pulmonary disease (COPD), fibrosis and lung cancer are a major burden globally. They affect one in five people in the UK alone, leading to more than 700,000 hospital admissions every year. An estimated 10,000 people are diagnosed with lung disease every week, but many more are living with significant undiagnosed and debilitating symptoms.
Lung disease can be difficult to diagnose: different lung conditions have similar symptoms, while shortness of breath may have other, non-pulmonary causes, such as heart disease. Patients may visit their family or hospital doctor several times before a diagnosis is made and are still at risk of receiving the wrong diagnosis, meaning that they may not receive the best treatment.
Patients with obstructive airway diseases such as COPD or asthma are particularly at risk from exacerbations: acute and potentially fatal deterioration of respiratory symptoms caused by inflammation. Patients are often hospitalised and require treatment with antibiotics and steroids. However, patients often struggle to identify the onset of an exacerbation, particularly as physical symptoms may come on suddenly. They may also have other comorbid conditions, so it is vital to identify whether current symptoms are due to an exacerbation of lung disease or other events such as acute coronary syndromes, worsening congestive heart failure, pulmonary embolism, or pneumonia.
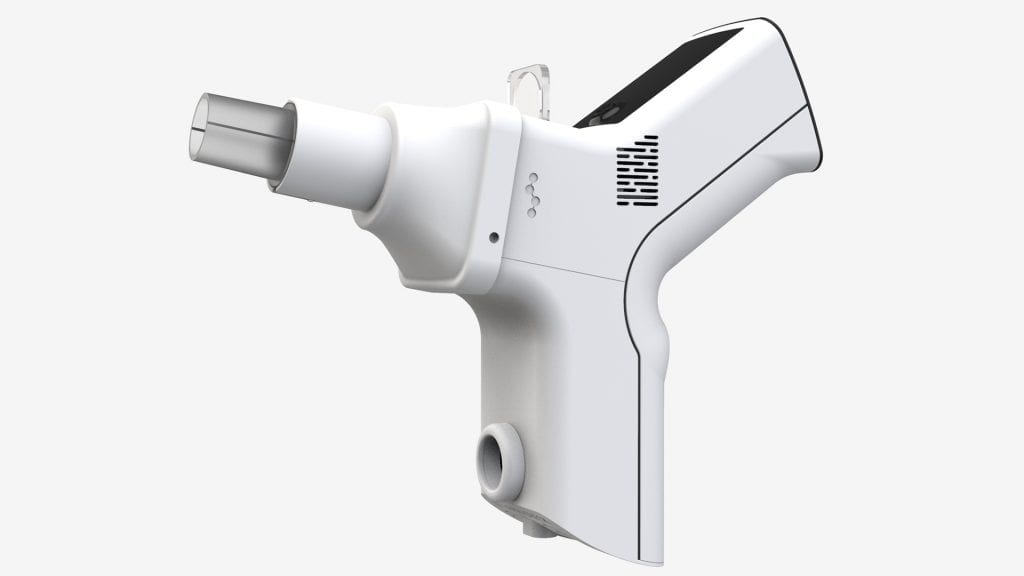
Inflammacheck provides a rapid screen for lung inflammation
The tests currently used to diagnose lung diseases require specialist equipment, such as spirometry, or specialist techniques, such as bronchoscopy. They are difficult or uncomfortable to perform, especially for people who are very short of breath, and may give poor or unreliable results.
Inflammacheck®, launched in 2019, is a new handheld point-of-care test which can quickly measure hydrogen peroxide levels in exhaled breath as a marker of inflammatory conditions in the lungs. The patient breathes normally through the device for three minutes; and the exhaled breath condensate (EBC) is collected and analysed within the device using a biosensor; and a result is provided within two minutes. Because only normal breathing is required, unlike in the case of spirometry, for example, the test is suitable for all patients, even those who present with shortness of breath.
Hydrogen peroxide levels are raised when there is inflammation and oxidative stress in the airways. It has been used for many years in research, but measurement has been too cumbersome for clinical use. Inflammacheck thus represents a step change in the diagnosis of airway conditions by enabling measurement of hydrogen peroxide at the point of care. Only minimal training is required to use Inflammacheck: the device is fully integrated and automated so that breath collection and measurement are seamless and do not require any sample handling; and the result is provided almost immediately. In addition to hydrogen peroxide content, Inflammacheck also measures carbon dioxide content, breath temperature, relative humidity and air flow. The combination of these different breath attributes is expected to be useful in diagnosis.
Trials with patients and healthcare professionals have shown Inflammacheck to be quick, reliable and easy to use, supporting healthcare professionals to rapidly identify active inflammation: an important first step in the diagnostic pathway.
The science behind Inflammacheck
During chronic lung inflammation, inflammatory cells such neutrophils, alveolar macrophages and eosinophils produce high levels of reactive oxygen species (ROS), resulting in oxidative stress. This can lead to further generation of inflammatory mediators and damage to epithelial cells, bronchial hyperreactivity and potentially aberrant growth of lung epithelial cells. (1) ROS are metabolised in cells to produce highly reactive oxidants such as hydrogen peroxide, which can be detected in EBC. (2,3) EBC hydrogen peroxide can therefore be used to measure the level of oxidative stress and airway inflammation. (4,5)
More than 200 studies have shown that EBC hydrogen peroxide levels are significantly higher in patients with COPD than in healthy patients and that levels rise further during exacerbations; there is also evidence that levels correlate with disease severity.4 Similarly, EBC hydrogen peroxide levels are significantly higher in (non-smoking) patients with asthma than in healthy subjects; (6,7) in moderate compared with mild asthma; in patients with neutrophil-predominant airway inflammation; (8,9) and in uncontrolled asthma compared with controlled disease and healthy controls. (10)
Whilst hydrogen peroxide is clearly a useful marker of lung inflammation, to date its measurement has required complex multi-step processing of collected breath samples, limiting its use to research settings. (3) Inflammacheck technology enables this important biomarker to be easily measured in the clinic.
Looking to the future
Hydrogen peroxide is a well-documented marker of lung inflammation, but has not yet been widely considered in clinical practice because there has been no suitable way to measure it. As a novel technology, Inflammacheck represents a major step forwards, bringing the measurement of hydrogen peroxide into the clinic. Clinical studies using Inflammacheck will enable the role of EBC hydrogen peroxide measurement in the diagnosis of airway disease to be fully explored and validated. As a rapid and easy-to-use device, requiring only minimal training to use, Inflammacheck can be readily incorporated into clinical studies without being time-consuming or burdensome.
The technology behind Inflammacheck also offers the opportunity to measure other constituents of EBC quickly and easily, including viruses and bacteria: the device can be used as vehicle to collect EBC, incorporating a biosensor directed at other compounds. In theory, the Inflammacheck device can be used to measure any chemical in EBC for which a biosensor can be developed. We are currently exploring the application in diagnosis of the ‘breath print’ provided by the Inflammacheck, combining hydrogen peroxide content and the four other breath characteristics recorded by the device.
CoronaCheck: demonstrating the adaptability of Inflammacheck technology
Exhalation Technology has recently developed the CoronaCheck™ biosensor for use with the Inflammacheck technology. EBC is collected using the Inflammacheck device; and the level of SARS-CoV-2 antigens is measured using an integrated biosensor, which can detect very low levels of the virus. As with the hydrogen peroxide measurement, the result is provided within five minutes at the point of care, without the need for intrusive nose or throat swabs, laboratory access or specialised staff. Thus, CoronaCheck has the potential to provide screening for COVID-19 in a wide range of environments such as hospitals, schools, primary care practices, drive-through centres, airports and sports arenas. Promising results from early studies with CoronaCheck are already available, and further studies are ongoing.
About Exhalation Technology Ltd
Exhalation Technology is a UK-based company, committed to developing simple and effective breath analysis devices for the diagnosis, monitoring and management of airways diseases. Exhalation Technology has developed the first rapid technology to measure hydrogen peroxide levels in EBC, launching the Inflammacheck device in Europe in 2019. The company has been able to use the Inflammacheck technology as the basis for rapid development of the CoronaCheck in response to the global pandemic.
References
1 Goldkorn, T et al. Antioxid Redox Signal 2014;21:2149-74.
2 Horvath, I et al. Eur Respir J 2017;49.
3 Konstantinidi, EM et al. ScientificWorldJournal 2015;2015:435160.
4 Kostikas, K et al. Chest 2003;124:1373-80.
5 Sugiura, H; Ichinose, M. Antioxid Redox Signal 2008;10:785-97.
6 Al Obaidi, AH. Ann Thorac Med 2007;2:18-22.
7 Teng, Y et al. Chest 2011;140:108-16.
8 Antczak, A et al. Arch Immunol Ther Exp (Warsz) 1999;47:119-26.
9 Loukides, S et al. Am J Resp Crit Care Med 1998;158:991-95.
10 Trischler, J et al. Respir Res 2012;13:14.
Helle Funch Nielsen
Exhalation Technology Ltd
www.exhalationtechnology.com
This article is from issue 16 of Health Europa. Click here to get your free subscription today.
























