Endocrinologist, Dr Frank Nobels explains why education around diabetic foot, and preventative strategies to mitigate the development of foot ulcers, are integral parts of diabetes care.
Chronic wounds may not be something we initially associate with diabetes. Yet, diabetic foot ulcers, whereby open sores or wounds occur on the feet, affect around 15-25% of diabetic patients and in extreme cases, ulcer-related complications can lead to leg amputation. Preventative and protective measures are essential to mitigate the development of difficult to treat wounds, including education around the signs and symptoms that both GPs and patients should be aware of. To find out more about common complications associated with diabetic foot care and what patients can do to protect themselves, Health Europa spoke with Dr Frank Nobels who is a professor in endocrinology and head of the diabetic foot clinic at OLV-Hospital in Belgium.
What makes people with diabetes more susceptible to slow-healing wounds? Can you outline some key risk factors?
There can be many reasons why wounds, in general, heal slowly in people with diabetes. If their blood glucose is very high, then their white blood cells struggle to function at the optimal level needed for efficient wound healing. Inadequate vascularisation of the skin, due to diabetic damage of blood vessels, is another factor. Skin edema, especially in the legs due to diabetic heart decompensation, can be another factor. But, in addition to poor wound healing generally, the healing of wounds at the level of the feet is especially challenging.
One in six people with diabetes will develop diabetic foot ulcers during their lifetime. Once they have the condition, the chances of recurrence are very high. Risk factors include diabetic neuropathy, whereby nerve damage occurs due to long-standing diabetes. As a result, patients feel less in their feet and cannot spot when their feet begin to hurt, or their shoes are starting to pinch. Where pain usually sounds the alarm to ensure someone no longer puts pressure on the affected area, loss of pain sensitivity often makes people with diabetes respond too late and continue to walk on the wound.
Vascular disease, whereby blood vessels narrow due to atheromatosis, is a known complication of diabetes. This reduces the oxygen supply, making feet more vulnerable and wounds less able to heal. A foot injury in diabetes can quickly progress unfavourably. Loss of viable tissue due to infection can turn a minor, manageable injury into a serious problem requiring long-term care and/or leading to loss of a large part of the foot or even to leg amputation. Many amputations could be prevented by shortening the referral time (‘time is tissue’).
Are there certain societal groups who are more susceptible to diabetic foot than others?
Certain societal aspects are important. If you are from a lower socioeconomic background, then your risk of developing a difficult to treat wound is much higher than if you are a highly educated person from a wealthier background, and typically more likely to understand the risk factors and how to mitigate them. Older people are also an at-risk group because often, they struggle to see and reach their feet. If you do not feel any pain due to neuropathy, then feet are even more distant, so you neglect them which can be problematic.
Are there protective lifestyle measures which people with diabetes can take to lower their risk of incurring complex wounds?
Good diabetes control and cardiovascular prevention (fighting obesity, getting enough exercise, not smoking, lowering cholesterol, treating high blood pressure) can, of course, prevent many problems. It is also important to have the feet examined at least annually. This can be done during a regular consultation with a GP, diabetes nurse or podiatrist and is not difficult.
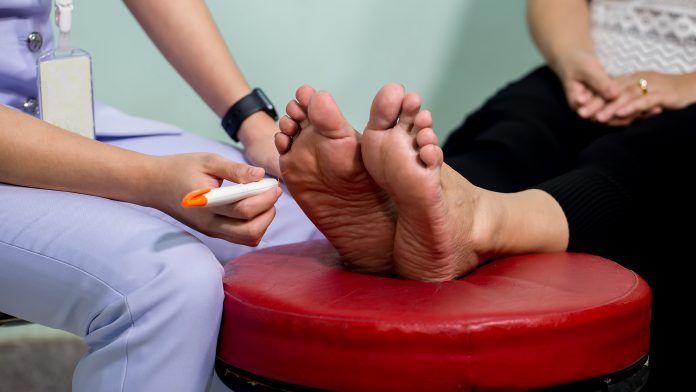
Sensitivity should be tested through touching with a monofilament which is a little wire that gives 10g pressure. You ask the patients to close their eyes, and you put the monofilament on their big toe, on the first metatarsal and the fifth metatarsal and if they do not feel at least two of the three, then they have neuropathy. Vascularisation should be checked by palpation of the foot arteries and skin, nails, and footwear should be inspected. All this can be done in a few minutes.
If there are problems, preventive measures can be taken which include wearing good socks and shoes. People with diabetes with feet at risk should be checking their feet daily and if they see that there is a lesion or a problem with their nails, they should seek help immediately. Of course, inspection of the feet can be difficult for older people. Asking a family member or nurse to check the feet regularly can solve this problem.
Reimbursement for suitable footwear for people that are at risk is also very important. If people lose feeling in their feet, they can be inclined to wear shoes that are too tight-fitting. Likewise, if they cannot gauge the temperature of their feet, they may put them near a radiator or burn them in the summer heat.
Are there improvements that could be made in preventing diabetic foot problems?
Prevention of diabetes is, of course, the most efficient way to avoid foot problems. Type 2 diabetes is unfortunately still increasing and the best way to prevent this is by learning about healthy living at an early age, making it a part of the school curriculum. There are many studies that show a link between a reduced rate of diabetes and green neighbourhoods with fewer fast-food outlets. Politicians should be shaping the environment to support healthy living. Early detection of diabetes is another important point. People should be made aware of the risk factors.
At the other end of the spectrum, once you have had a diabetic foot ulcer your risk of recurrence is very high, especially if you have already lost a toe or part of the foot. These people need to see their podiatrist regularly and have a prescription for suitable footwear. Unfortunately, people often change their appropriate footwear to slippers when they go indoors, but these do not give enough protection and are often the cause of wounds. We need reimbursement for indoor as well as for outdoor shoes, as is already the case in the Netherlands.

How could digital technology be employed to stimulate behavioural changes and help patients to better monitor their symptoms?
There is early research on scales which can measure the temperature of the feet. A region of the foot with an elevated temperature could be the beginning of inflammation and an ulcer. In the future, we believe there will be more technology to help people, such as smart socks and tools that sense if shoes are being worn correctly and alert the wearer if there is too much pressure.
The concern here is how these technologies can be made accessible to all, as opposed to only wealthy populations. We also need to consider how older adults that need them most, but are often the least familiar with apps, can be reached.
Can you highlight any innovations in wound care that have helped alleviate or mitigate chronic wounds for diabetic patients?
What has made a big difference over the years is the introduction of diabetic foot clinics. It is often thought that you can heal a wound by applying the right wound product. However, with diabetic feet this is definitely not enough because they must carry pressure and wounds cannot heal if we are constantly walking on them. Another problem is inadequate vascularisation.
Here the expertise of a multidisciplinary diabetic foot clinic team is needed. Techniques of offloading the ulcer are applied, such as special walkers or wound shoes, or if possible, a total contact cast. This cast forms a shell around the shape of the lower leg and foot, maximally decreasing pressure over the wound area. Very often we see that in such a cast, in a few weeks, the wound has healed without any product being applied, just by offloading.
Adequate revasculariation is another essential component of the treatment. The technology to obtain better vascularisation, even in the small vessels of the feet, has really exploded in the recent years allowing us to save many legs.
So, we have a lot to offer people with diabetic feet, but the earlier we treat them the better. Unfortunately, too much time is often lost by trying to heal the wound with wound products, without thinking about offloading or revascularisation. Waiting too long can lead to infection, loss of tissue and even amputation. Early referral is therefore, extremely important.
Frank Nobels, MD, PhD
Professor in endocrinology at OLV Hospital,
Aalst (Belgium)
This article is from issue 20 of Health Europa Quarterly. Click here to get your free subscription today.






















