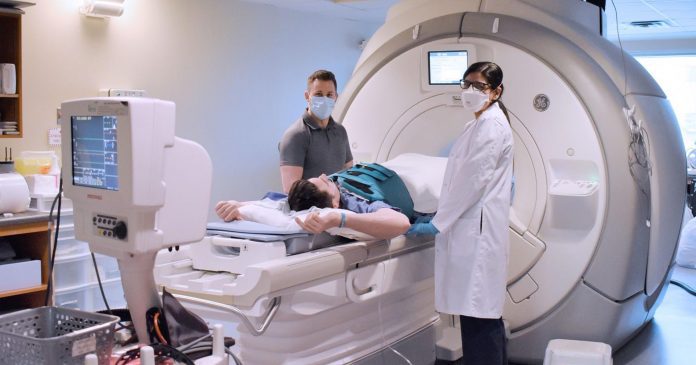
An innovative lung-imaging technique developed by Western University shows what potentially causes long Covid symptoms.
Long Covid has been widely reported, and sufferers report symptoms of brain fog, breathlessness and fatigue months following infection. Researchers have identified for the first time that using a functional MRI with inhaled xenon gas shows that long Covid symptoms are related to microscopic abnormalities that affect how oxygen is delivered from the lungs to red blood cells.
“I think it is always a conundrum when someone has symptoms, but you can’t identify the problem. Because if you can’t identify the problem, you can’t identify solutions,” said Parraga, Tier 1 Canada Research Chair in Lung Imaging to Transform Outcomes at Western’s Schulich School of Medicine & Dentistry.
The largest MRI study of long Covid symptoms
The LIVECOVIDFREE study’s findings were published in Radiology and are the first to a potential cause of long Covid symptoms.
The participants inhaled polarised xenon gas whilst inside the MRI; this illuminated in real-time the function of the 300-500 million tiny alveolar sacs that deliver oxygen to the blood.
“With our MRI technique, we can watch in real-time the air moving through the alveolar membrane and through to the blood cells; and we can actually see the function of the tiny alveolar sacs in the lungs,” said Parraga. “What we saw on the MRI was that the transition of the oxygen into the red blood cells was depressed in these symptomatic patients who had had Covid-19, compared to healthy volunteers.”
“Some patients remained symptomatic for up to 35 weeks.”
The researchers recruited patients with suspected long Covid from two hospitals in London, Ont. – London Health Sciences Centre’s (LHSC) Urgent Covid-19 Care Clinic (LUC3) and St. Joseph’s Health Care London’s post-acute Covid-19 program. Participants included those with shortness of breath more than six weeks post-infection, with some remaining symptomatic after 35 weeks.
CT scans illuminated the ‘abnormal trimming’ of the vascular tree, pointing towards an impact on the tiny blood vessels that deliver red blood cells to the alveoli to be oxygenated.
The study appeared to show no difference in the severity of this abnormality between hospitalised patients and those who recovered without hospitalisation. “For those who are symptomatic post-Covid, even if they hadn’t had a severe enough infection to be hospitalised, we are seeing this abnormality in the exchange of oxygen across the alveolar membrane into the red blood cells,” said Parraga.
Study co-author Dr Michael Nicholson is a respirologist with St. Joseph’s post-acute Covid-19 program, a former member of the LUC3 clinical team at LHSC, and an associate scientist at Lawson Health Research Institute. He said patients describing these symptoms were also showing normal results on clinical breathing tests.
“We were looking for further modalities to look at their lung function that were not found through traditional clinical testing,” said Nicholson. “The findings allowed us to show that there was a physiological impact on their lungs that correlated with their symptoms.”
























