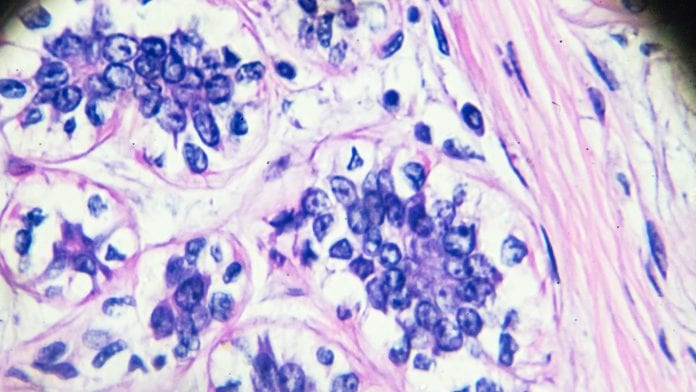
New research has presented a new and more accurate method of predicting long-term outcomes for ductal carcinoma and has confirmed the role of the oestrogen receptor biomarker in this type of pre-invasive breast cancer.
Oestrogen receptor (ER), a type of protein that is expressed in some breast cancer cells, is routinely tested in invasive breast cancer to predict long-term outcomes and select treatment options, however, its role in ductal carcinoma in situ (DCIS) has been previously unclear. However, this new research confirms the role of ER in predicting long-term outcomes in DCIS.
In the study by Queen Mary University of London, published in Clinical Cancer Research, the authors report a new and more accurate method to evaluate ER for predicting long-term outcomes in DCIS.
Oestrogen receptor
ER is not generally evaluated in this pre-invasive stage of breast cancer and this study is the first to use samples to investigate ER as a prognostic marker in DCIS.
The researchers observed multi-clonality in ER expression in 11% of ER-positive DCIS (ie: ER-positive DCIS with distinct ER-negative clones) and investigated the prognostic role of such multi-clonality in ER expression, finding that ER is a strong prognostic factor with greater than three-fold risk of ipsilateral recurrence in ER-negative DCIS.
Lead author Mangesh Thorat, Queen Mary University of London, said: “It is unlikely that such a study could currently be reproduced elsewhere in the world, and the robustness of these results means we can rely on them to make changes to clinical practice. Routine testing of ER in DCIS will help to avoid both overtreatment and undertreatment in this type of breast cancer. The insights from this study will also help improve future breast cancer research through use of new scientific models, particularly in areas of drug resistance and the use of targeted therapies.”
Michelle Mitchell, chief executive of Cancer Research UK which contributed to funding of the study, said: “It’s currently very difficult to determine whether DCIS will develop into invasive breast cancer, meaning thousands of people undergo unnecessary and intense treatment. This research shows that in the future we might be able make sure patients are getting the right care, potentially saving many from undergoing cancer treatment that is both physically and mentally demanding.”






















