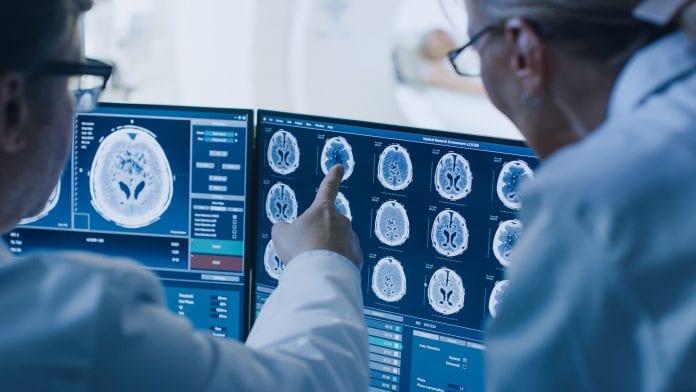
A new breakthrough could pave the way for therapies to treat rare childhood brain disorders by helping us to understand how they develop.
Findings from the new study, conducted by the University of Sheffield, have revealed that defective immune cells in the brain contribute to the development of these rare neurological diseases – known as leukodystrophies. Results from the study, published in the journal Glia, suggest that the disorders start during brain development in pregnancy.
Currently, around one in 7,600 children are affected by these disorders however, there are very limited treatment options for them.
Leukodystrophies
The discovery by academics from the University’s Neuroscience Institute and Bateson Centre has revealed that defective immune cells in the brain called microglia contribute to the development of leukodystrophies.
Leukodystrophies are a group of rare neurological diseases that cause severe physical and mental disabilities in children. One in 7,600 children are affected by the disorders which include symptoms that usually appear in the first year of life and get progressively worse as the child grows older.
Paving the way for future therapy
The results from the study could be used to help pave the way for the development of better therapies in the future.
Nearly half of our neurons die during the formation of our brain throughout pregnancy and it is the role of microglia to clear them away.
The researchers used transparent zebrafish models to directly observe how brain cells develop and found that the microglia were impaired when trying to clear away the dying neurons in the brains that went on to develop a leukodystrophy.
Dr Noémie Hamilton, European Leukodystrophy Association (ELA) Research Fellow at the University of Sheffield, said: “The first and main challenge for microglia during brain development is to clear away dying neurons. We found that in our zebrafish model of human leukodystrophy, deficient microglia failed to digest dying neurons. Cells digest their content using their lysosomes which are an acidic cellular compartment used as a recycling factory. We showed that our zebrafish model had lysosomal defects, blocking microglia from performing normally.”
Animal models of leukodystrophy are rare and often don not look like the human pathology, as they lack the characteristic brain abnormalities and movement problems seen in human patients. However, researchers have created the first zebrafish model for human leukodystrophy and have shown that this model had similar physical and brain anomalies to patients.
Dr Hamilton continued: “This was associated with an inflammatory response which could damage the brain and be the start of the pathology of the disease.”
The study highlights that focussing on early dysfunctions during brain development and their consequences will provide a better understanding of these rare devastating diseases.






















