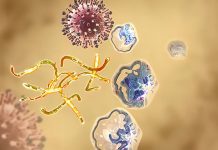
For the first time, scientists have discovered that mouse and human lymphatic endothelial cells use primary cilia which may direct the growth of a functional lymphatic network.
The new research carried out by researchers at South Dakota State University and the University of Massachusetts Medical School have found that the lymphatic endothelial cells (LECs) – which make up the inner and outer lining of lymphatic vessels – use primary cilia.
The team believe that LEC primary cilia may direct the growth of a functional lymphatic network, not only during prenatal development, but also throughout life during inflammation and wound healing, and in response to cancer.
The findings, which have been published in the open-access journal Frontiers in Cell and Developmental Biology, could lead to new medical applications.
Lymphatic vessels
The study shows that primary cilium, an antenna-like subcellular structure, or organelle, protruding from the outside of many types of vertebrate cells, has an important role in guiding the growth of lymphatic vessels.
The findings show that mice, in which the formation of primary cilia in LECs is prevented, develop lymphatic vessels that are locally overgrown. The team say this suggests that signals received by primary cilia may guide proper lymphatic vessel growth patterns.
Corresponding author Dr Darci M. Fink, an assistant professor at the Department of Chemistry and Biochemistry of South Dakota State University, said: “The first images were so exciting. LECs do have primary cilia and they are clearly important for patterning growth. The finding of a new regulatory ‘hub’ on LECs means that the way we think about how and what kind of signals are received by these cells has fundamentally changed.
“Targeting the assembly of cilia by the cell or their ways of signalling could allow us to control or stimulate lymphatic vessel growth in new ways.”
The lymphatic vessel system of vertebrates consists of hundreds of lymph nodes connected by a network of vessels spread throughout the body and these vessels play a crucial role in health and homeostasis. They facilitate immune cell traffic during inflammation, drain excess fluid from the space between cells to lymph nodes and return it – clear of pathogens – to the bloodstream, and absorb fat molecules as an energy source.
These cells first appear during embryonic development, but ‘lymphangiogenesis’ – the growth of new lymphatic vessels – continues throughout life in an adaptive response to the microenvironment, particularly during inflammation and wound healing. Faulty lymphangiogenesis can cause edema, impaired wound healing, chronic inflammation, and tumour progression.
“Primary cilia are such an essential part of the function of many cell types, including those that form other tube-like structures like blood vessels, breast ducts, and kidney tubules. Now we can add lymphatic endothelial cells to that list. Understanding exactly how primary cilia govern LEC movement, division, and tube formation and how to exploit these mechanisms is the next exciting challenge,” says Fink.
The team used microscopy to show that in tissue from healthy mice, primary cilia on LECs can protrude either from the outside or the interior cavity, and that the incidence of primary cilia is also particularly high on LECs at the tips of growing lymphatic vessels, where guiding cues are received. The team say this suggests that LECs might use their cilia to interact with the microenvironment inside as well as outside lymphatic vessels, for example sensing flow or the presence of soluble signalling molecules.
Disturbed development and the role of lymph vessels in disease
The team also found that the presence of a functional cilium on embryonic LECs is necessary for the healthy prenatal development of the first lymphatic vessels. To show this, the team used a genetic ‘cut-and-paste’ tool to create a new transgenic line of mice, in which the key gene IFT20 – necessary for the molecular assembly of cilia and transport of proteins as ‘ciliary cargo’ – can be deactivated. As predicted, the majority of LECs from these mice lacked a primary cilium and the embryos showed significant edema.
The lymphatic vessels of the embryos were also dilated and improperly branched, became surrounded by excess smooth muscle, and inappropriately contained red blood cells meaning that the presence of a functional cilium on embryonic LECs is necessary for the healthy prenatal development of the first lymphatic vessels.
The team studied the importance of primary cilia for guiding lymphangiogenesis in adult mice, during inflammation, wound healing, and tumour growth.
To cause localised acute or recurrent inflammation, they used the so-called cornea inflammation bioassay where small synthetic sutures are inserted (under anaesthetic and continuous pain control) in the cornea of the eye. This procedure is known to stimulate LECs present in lymphatic vessels at the edge of the cornea to sprout, divide, and migrate toward the inflamed area, forming new lymphatic vessels.
The team found that the process was faulty in mice without the IFT20 gene, where the network of new vessels became overgrown: too dense and with too many branches. The authors conclude that in the absence of primary cilia, lymphangiogenesis in response to disease is poorly regulated and results in new lymphatic vessels that are not properly patterned.
Coauthor Prof Gregory J. Pazour, University of Massachusetts Medical School, said: “The striking overgrowth of lymphatic vessel seen after the loss of primary cilia points to the key role of cilia in co-ordinating the physiology of LECs with their microenvironment.
“The challenge now is to identify the signals sensed by lymphatic cilia. Across eukaryotic organisms, cilia are known to use a wide range of signals such as small molecules, peptides, physical forces, osmotic changes, and light, so in principle lymphatic cells have many options for sensing.”