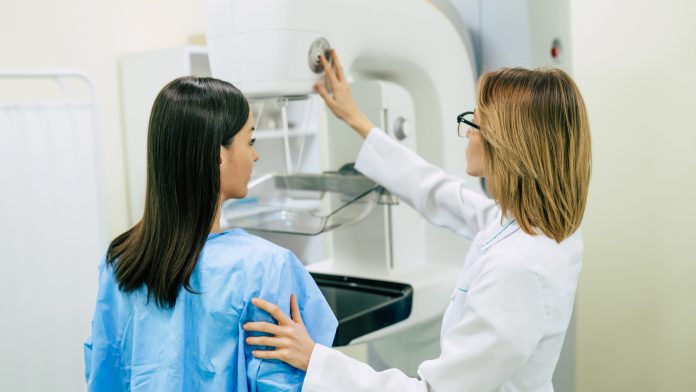
The NHS has announced a record number of people who received cancer checks in the last 12 months, the highest year recorded.
Cancer checks are vital for detecting the disease at the earliest stage, allowing for the best treatment options. Cancer checks can include cervical, breast and bowel cancer screening. Despite a record number of cancer check referrals, NHS cancer chiefs continue to encourage people to come forward for screening.
Data illuminates that during the Omicron COVID-19 wave, cancer checks for suspected cancer were at 116% of pre-pandemic levels, with around 11,000 people getting checked every day over the last year. Additionally, during the COVID-19 pandemic, the number of people being treated for cancer remained higher than before the pandemic – with 315,000 starting treatment compared to 313,000 before the pandemic.
How did the NHS achieve the record number of cancer checks?
To accomplish this milestone, spending on awareness campaigns for cancer checks has been doubled and health chiefs continue to encourage people to come forward if invited by the NHS or if they have experienced worrying symptoms.
NHS services across the country have expanded their diagnostic capabilities through one-stop shops for tests, mobile clinics and cancer symptom hotlines, ensuring people are diagnosed and treated as early as possible to give them a much better chance of beating the disease.
More than 30,000 people every month are being invited for lung cancer checks through NHS mobile trucks that are visiting at-risk communities across the country, as part of the biggest programme to improve early lung cancer diagnosis in health service.
Another intervention kicked off in London, where the ‘Man Van’ scheme was launched by The Royal Marsden NHS Foundation Trust, RM Partners West London Cancer Alliance, and The Institute of Cancer Research, London. It aims to provide free health checks for men and boost early diagnosis of prostate and other urological cancers.
The Rotherham NHS Foundation Trust has introduced telephone triage for certain cancer referrals so that patients can speak to doctors sooner, as well as increasing the use of ‘straight-to-test’ pathways for lower gastrointestinal patients to get diagnosed as early as possible and expanding one-stop-shop slots for patients referred under a breast cancer pathway, so patients can get all their tests in one trip.
Managing cancer during COVID-19
The NHS aimed to maintain cancer treatment for patients and since the start of the COVID-19 pandemic in March 2020, more than 4.7m have been referred and more than half a million people have started treatment.
Professor Peter Johnson, NHS England National Clinical Director for Cancer, said: “We know the pandemic meant that at first, we saw fewer patients, but in the last year GP’s have been referring people for investigation in record numbers and have been working hard to make sure people with worrying symptoms can be seen. The NHS has continued to prioritise cancer care throughout the pandemic.
“It’s vital people continue to come forward, so if you have a sign or symptom that you’re worried about, such as a persistent cough that is not COVID, or prolonged discomfort in the abdomen, please come forward – getting checked out could save your life”.






















