Dr Richard Gilpin, Specialist Registrar in Geriatric Medicine and member of the Doctors’ Association UK editorial board, discusses the current challenges facing urgent care delivery in the UK.
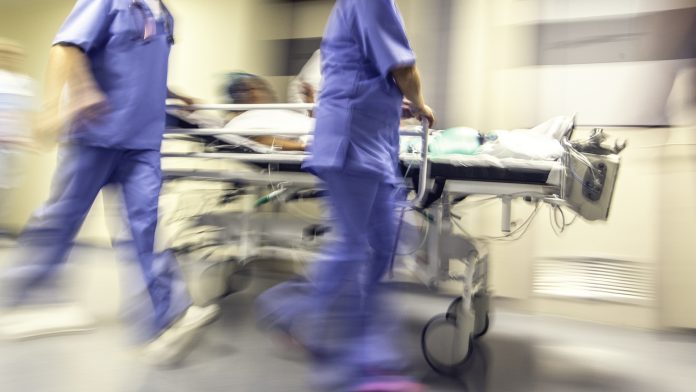
It is not difficult to describe the current crisis in delivering urgent care in the UK. Waits in Emergency Departments (ED) are up, with only two-thirds of patients seen within the mandated four hours. Ambulances queue outside departments, with patients sometimes spending over 24 hours in crowded waiting rooms. Doctors cannot deliver the urgent care they need to, leading to moral injury and burnout.
The often-cited cause of problems in emergency departments (ED) is ‘exit block’; not enough space in the hospital to move patients to beds and not enough care in the community to expedite the discharge of patients who need it. These patients are typically the frail elderly. The Get it Right First Time (GIRFT) report on Geriatric Medicine describes how less than 10% of ED attendees are over seventy-five, but they occupy over 20% of bed days. If you are over 75 and attend ED for any reason, there is a 40% chance you will be admitted to the hospital. Nearly half of these admissions are for longer than two days.
Of course, this trend cannot continue. A report from the Royal College of Emergency Medicine describes how it has ‘become normalised for ED to soak up risk and continue accepting patients in a manner not expected in any other part of the NHS’.
Intermediate care
The GIRFT report highlights that for many patients, a patient-centred approach could avoid hospitalisation. This involves greater use of services under the umbrella term ‘intermediate care’. Essentially, intermediate care is a hinterland between primary and secondary care, beefier than your local GP but with no need for being wheeled through the emergency department. It is time-limited care – typically less than six weeks and typically in your own home – and involves a team of carers, therapists, nurses, and other specialists tasked with supporting your recovery. According to a case study published via the National Institute for Health and Care Excellence, over half of older adults who had a short stay in hospital could have potentially been managed in the community.
Intermediate care is certainly not new; it was developed as part of the NHS Plan in 2000. However, it still feels that intermediate care is the exciting promise of modern healthcare. At its best, the sick patient remains in their own home with a raft of therapists and carers are there to support; doctors and nurses are there to diagnose and treat, with access to blood tests, intravenous antibiotics (antibiotics given through a needle into a vein) and even oxygen. Carried out well, the clinician feels like they are doing positively, and the patient feels well supported in their own comfortable bed rather than a trolley in a noisy and crowded emergency department.
It is worth noting that for some, the GIRFT report makes difficult reading due to the level of anti-hospital sentiment in the piece. For example, there is no doubt that a patient who falls and sustains a hip fracture will need to go to the hospital. Thanks to national audits, improvements in care have resulted in a 30-day mortality reduction from over 11% fifteen years ago to less than 7%. If a patient needs an X-ray, scan, or 24-hour monitoring, this cannot be carried out at home. Sometimes a hospital is the best place, and sometimes it is the only place. Framing the frail elderly as not appropriate for the hospital or wasteful of its resources risks alienating the group of people who often gain the most benefit from being there. Thankfully, the ‘bed blocker’ terminology has largely gone, but the sentiment often remains, and other terms are still commonly used. A patient who returns to the hospital having just been allowed home is a ‘failed discharge’ – who is it who has failed? The previous hospital team? The patient?
If we agree that a cohort of patients may be better avoiding ED, then how do we achieve the GIRFT recommendation of avoiding inappropriate hospitalisation for the frail elderly? If the NHS is Disney, then emergency departments are Mickey Mouse – the instantly recognisable figurehead. How will anything else ever compete?
Avoiding the emergency department
We need to develop a clinician-centred approach to these interventions. How does one access help that does not entail hospital admission? Does it require less administrative burden than arranging an ambulance? The GP Worklife survey released earlier this year reported that three-quarters of GPs had considerable or high pressure from paperwork, the fourth-highest job stressor. Any extra burden placed on clinicians should involve less ringing around and form filling.
Hence the other advantage of ED – it will always be there. The problem with sustaining intermediate care services is linked to realising the funding. A new service promises to reduce admissions or length of stay and offset the cost of the service, and when this is not realised, cuts are made. Now, it may be that services do not deliver, that the service provides resilience against the new demands placed on it, or that it works in more subtle ways which are difficult to measure, like reduced carer burden or improved quality of life for patients.
Whatever the outcome, services that are patchy and short-lived are cruel to both the patients and the clinicians that put their confidence in them. The GIRFT report appears to suggest that intermediate care will result in an overall saving to the health system; however, this may not be the case. In 2017, the Social Care Institute for Excellence reported that ‘Care outside of a hospital generally is unlikely to be cheaper for the NHS in the short to medium term’. And it is clear to see why. The hospital provides an economy of scale that community care cannot realise.
At the start of the pandemic, there were numerous changes across the health system. Intensive care and emergency medicine departments were understandably supported, whereas elective care was scaled back or stopped. Intermediate care often became more limited, typically from a combination of community staff supporting the hospital and increased rates of sick leave. When the next pandemic arrives and another health crisis unfolds, will these services still exist?
There is also the problem of staffing. There is not the capacity to be creating new teams at present. Many departments operate with gaps in nursing and doctor numbers. A care assistant working for an intermediate care team is likely to be paid less than in their local supermarket or pub, with far less physical demand and responsibility. For this to work successfully, we need to be paying our care workers more.

Intermediate care is a hinterland between primary and secondary care, beefier than your local GP but with no need for being wheeled through the emergency department
Risk
Of course, if we aim to move people away from using their local emergency department, the risk is shifted elsewhere.
Doctors are well used to dealing with risk. The twenty-year-old you saw with chest pain after working out, this could be a heart attack, blood clot or a myriad of other life-threatening problems; we realise the risk of this is so low that usually reassurance, pain relief and advice about if it worsens will suffice. Talking about risk is addressing the simple question: will my actions cause harm to this patient in front of me? A survey we completed in our local emergency department showed that for the patients over sixty-five, half of them had been sent in by a healthcare professional. This extended beyond a patient’s GP and included pharmacists, dentists, and opticians; one patient reported their husband’s dialysis nurse suggested she attend ED to get checked out. And you can see why the idea of going ‘to the Emergency Department, just to be safe’ is pervasive. Your typical emergency department is open all day and guarantees you review and urgent care by a clinician.
And of course, hospitals are not safe places; one-third of frail patients will lose some of their ability to look after themselves during a hospital stay, and many will develop nutrition and swallowing issues. Inpatients are more likely to fall or develop pressure ulcers and hospital-acquired infections. The pandemic changed the landscape of hospital care further – clearly demonstrating to the public that there was a risk to entering those bright doors of catching a disease; ending up in a worse state than when you started. Many patients got infected with COVID in hospital, and many died.
It is common for doctors to practice what is termed defensive medicine – the ordering of treatments, tests, and procedures to protect the doctor from criticism rather than diagnose or treat the patient. According to a 2013 study published in BMC Medical Ethics, over half of doctors report making an unnecessary referral to a specialist from practicing defensively. When you have a patient that appears to need urgent care, the fear of making a career-ending mistake influences your every decision.

We need to develop a culture that rewards appropriate clinical judgement in a system where clinicians feel safe to make appropriate decisions above acting defensively
What next?
Emergency departments cannot continue to be flogged the way they have been, and we need to be thinking of better ways of treating our most vulnerable when they need help. No one wants patients held in the back of ambulances, in trolleys in corridors, or diverted to another hospital miles from their home. The alternative should be easily accessible, adequately staffed and sustainable long term. But we also need to develop a culture that rewards appropriate clinical judgement in a system where clinicians feel safe to make appropriate decisions above acting defensively.
We also need to be listening to our patients. It is not uncommon for patients to refuse to come to the hospital, sometimes multiple times before coming in. Urgent care can be seen as all or nothing – go to ED or not. The patient needs to be aware of what the options are and what risks are involved. When it comes to the crisis in urgent care, safe alternatives to hospitals are essential.
Dr Richard Gilpin
Specialist Registrar in Geriatric Medicine
DAUK Editorial Board
https://www.dauk.org/
https://www.linkedin.com/company/thedoctorsassociationuk/
https://www.facebook.com/TheDoctorsAssociationUK
https://www.instagram.com/accounts/login/?next=/TheDoctorsAssociationUK/
https://twitter.com/theDA_UK
https://www.youtube.com/channel/UC-88cPTN9lT5rDFocn2GywQ
This article is from issue 22 of Health Europa Quarterly. Click here to get your free subscription today.