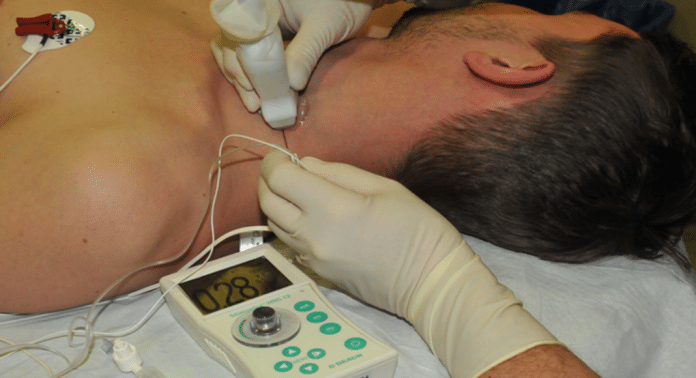
Dr Sermeus of the Department of Anesthesia, Antwerp University Hospital, explores the evolution of regional anesthesia and the impact of technology on its development.
Since the first general anesthesia (GA) with ether by W. Morton in 1846, anesthesia has seen a rapid evolution. In tandem with advances in pharmacology, anesthesia techniques were developed to facilitate surgical procedures and to increase patient safety. Besides GA, regional anesthesia (RA) was introduced in the late 19th century when K. Koller used cocaine as a local anesthetic and W. Halsted performed the first peripheral nerve block (PNB) by infiltrating a local anesthetic (LA) solution around the nerve, making transmission for sensation and pain impossible.
Since then, a fairly rapid evolution occurred in RA with the description of different PNBs, but also the spinal and epidural anesthesia. These RA techniques were, in the beginning, used as the sole anesthesia for surgery. But later on, RA and GA were used in combination in difficult and long-lasting surgical procedures with concomitant extreme post-operative pain. The RA technique was then used for postoperative analgesia which, being very effective, decreased the use of systemic analgesics, like morphine and non-steroidal anti-inflammatory drugs, which are known to have important side effects.
Advances in pharmacology, electronics and imaging techniques pushed the research in PNB to high levels and for use in daily practice. Soon some drawbacks appeared. All LA is limited in time, with the longest duration lasting between ten and 15 hours, as well as being limited in dose, due to toxicity. Evolution in clinical practice for efficacy and safety made the use of high-tech equipment inevitable. Security and privacy concerns made, and still make, research more complex. And, last but not least, financial limitations increased in prevalence. On one hand, for governments and insurance companies the sky is not the limit in regard to health care, yet financial support for research is getting more and more difficult.
Anatomy: the base of regional anesthesia
Since Andreas Vesalius, anatomy hasn’t change a lot, with the exception of microscopic anatomy (histology), which is of less concern in anesthesiologists’ daily practice. Without thorough knowledge of anatomy, it is impossible to perform RA. For some years now, research in chronic pain has focused on the interaction between the two nervous systems of the human body and, more specifically, the modulation of the autonomic system on the somatic nervous system. Some research has been done in acute pain with the same idea, namely the interaction of both nervous systems on the perception of postoperative pain.
Advances in pharmacology
After the first use of cocaine in 1885, many different LAs made their appearance. Short-acting drugs, which were used for short and not too invasive surgical procedures, either by infiltration of the surgical site or for PNB at distance of the surgical site, had an active effect of a few hours. Later, the discovery of long-lasting LA changed mainly post-operative analgesia, due to their active effect of several hours. Even when used in lower concentrations, reducing motor block and anesthesia, they were very efficacious for pain relief. The other side of the coin is that these long-lasting drugs were more toxic and increasing infiltration volume and dose were obsolete. A solution for an even longer pain relief treatment after major surgery was found with the use of catheters and continuous infiltration of LA around the nerves for the duration of the postoperative pain. This meant new material, better skills and higher costs.
Another way to increase duration and efficacy was by mixing another drug with LA, which would have an additive effect and increase both duration and anesthetic effect of the LA. Of course, none of those mixed solutions could last as long as continuous infiltration by means of a catheter. For many years, lots of studies were performed in this way with all possible drugs as additives. The main issue was that none of these drugs were ever synthesised to be injected outside the blood stream and, as a matter of fact, adding them to LA for a PNB was an off-label use. The main reason for this was the risk of neurotoxicity. Use of off-label products in clinical practice is a very controversial topic. Firstly, no performed studies with additives made their use for PNB legal. However, some are accepted as common practice due to their widespread use in many studies. Secondly, journals are not inclined to publish new articles on off-label drugs, making future studies on this topic difficult.
Advances in imaging
Over the last 50 years, anesthetic blocking techniques have evolved due to expanding knowledge, the development of equipment and the introduction of peripheral nerve stimulation and ultrasound. In the beginning, PNB was performed by eliciting a paresthesia – an electrical current in the nerve, similar to that experienced when hurting the elbow, resulting in an electric sensation reaching the hand – by touching the nerve with a needle, localising the nerve. This sensation confirmed the needle tip position was close to the nerve. This technique had a risk of creating a (small) lesion to the nerve.
From the seventies onwards, a nerve stimulator was used which stimulated the nerve with a small electric current in order to locate and identify peripheral nerves. In this technique, a special, insulated needle with a conductive tip was used, in conjunction with a small, battery-powered nerve stimulator. When the needle tip lay close to the peripheral nerve, the electric current escaping through the tip induced a distal motor response in the respective muscular distribution of the nerve. Thus, the nature of the muscle contractions made identification of peripheral nerves possible. Furthermore, the proximity of the needle tip to the nerve could be assessed in terms of the intensity of the electric current used to elicit the response – the lower the current required, the closer the needle tip to the nerve. Now, with the use of ultrasound, this technique is used to reduce the risk of intraneural penetration of the needle.
The paresthesia, as well as stimulation techniques, had several disadvantages. However, both of these landmark-guided techniques, where the anesthesiologist determined his puncture site by looking at external anatomical characteristics on the skin or by palpation of different structures such as arteries or bony structures, were “blind” techniques.
Occasionally, localisation of nerves could be difficult due to anatomical variation, or lack of information on nerve depth, relative to the skin and these techniques were dependent on fully functioning nerves.
In 1994, S. Kapral was the first to describe the use of ultrasound for detecting nervous structures and to visualise the injection of LA solution around nerves. These advantages, namely, visualisation of the anatomy, the needle and the spread of the LA improved block success rate. Unfortunately, the notion that ultrasound would resolve all of the difficulties in performing PNB was an illusion and the limitations of the technique quickly became apparent. The belief that ultrasound could decrease or even abolish direct needle trauma to the nerve, by means of direct observation of structures during needle advancement and injection in real time, has not been upheld. As a consequence, research was focused on techniques for avoiding nerve lesions when using ultrasound. Soon, guidelines for performing PNB appeared for reducing the risk of nerve trauma. Avoiding this risk would have been better, but with the actual knowledge and technique, this seems impossible and further research has to be done.
Advances in PNB evaluation
For many years, and still used in clinical settings, nerve blocks were evaluated by a pinprick test or with cold sensations to ether, both of which provided a binary answer. These two methods have the advantage of being fast and easy to apply, however, they are subjective, not gradual, and are dependent on the intensity of the application. In our department, we used a novel and repeatable technique to objectively, reliably and gradually assess the anti-nociceptive intensity, duration and extension of the applied nerve block, namely, thermal quantitative sensory testing (QST). This technique separately tests all the nerve fibres involved in nociception with their spinal and central processing, and is used for testing neuropathies in chronic pain cases. We assumed that injection of a LA around a nerve would create a (reversible) neuropathy that could be gradually evaluated with QST.
Moreover, if for any reason the injected solution would have been toxic to the nerve, this could be diagnosed with this evaluation technique as well, measuring an incomplete recovery. This tool is actually the most advanced evaluation technique for research on efficacy of PNB in research conditions, independent of which LA is injected, or if any LA is used.
Evolution in social security and the financial consequences
In Europe, and anywhere in the world, people want the best medical care. Technical, especially the electronic evolution, and actual research in pharmacology and pathology have opened a lot of possibilities in medical care for diagnosing and curing pathologies. RA hasn’t fallen behind in this evolution yet has, however, developed at a slower pace, since research grants are mainly focused on health problems like cancer or for developing new cures.
The drawback of this evolution is ethical and financial. Ethically, do we have to treat every patient, even if life expectancy is reduced to a minimum? It is impossible to answer this in a few sentences and this is not the subject of this report. However, keeping patients in pain after a surgical operation, with the risk of inducing chronic pain, is neither ethically nor financially acceptable.
The financial issue is even more prevalent, as governments manage an increasing population which is getting older and with more and more severe health problems. The technical evolution hasn’t made medicine cheaper, on the contrary. So, governments facing a low-economic conjuncture make restrictions in their social security budgets. Decreasing hospital costs, then, seems to be the only solution. In anesthesia and surgery, this means reducing equipment expenses, but more importantly, reducing hospital stay duration after surgery. For most cases, reducing budgets means patients leaving hospital in pain and with a real risk of inducing chronic pain syndromes, which will increase costs further. PNB with a catheter is of course a possibility, but more expensive for two reasons: firstly, more equipment; and secondly, sending a patient with a catheter still leads to mandatory care at home. The only possibility seems to be a single shot PNB with a very long-acting local anesthetic and with minimal motor blockade.
Future research in regional anesthesia
When taking these advances into account, it is quite obvious that RA has progressed over the decades. More specifically, visualisation of nerves and the relevant anatomy, by means of ultrasound, has improved safety and success rate. On the other hand, safety issues regarding nerve lesion, due to the needle and/or the direct injection into the nerve or due to the toxicity of LA and /or additives, appeared to be some of the main concerns. However, some financial issues in social security systems might push research to other forms of pain relief, especially postoperative analgesia. Research on new catheters and patient-controlled infusion systems for LA could have come to an end, owing to their cost and cumbersomeness.
Some research has already appeared on a very long-acting LA with some success, however this is not yet convincing. The same is true for the interaction between the different nervous systems of the human body, but this research is still in its infancy. Moreover, new techniques might block a nerve without the use of LA agents. These new nerve blocks could be variable over time and be modulated to the needs of analgesia. Future research has to focus on these new possibilities in the next few years.
Whatever drug or technique not involving LA solutions is used to block nerves in RA, the efficacy of all could be tested in an objective manner. Meanwhile, the neurotoxic effects or even direct lesions to nerves, regardless of size, could be detected with thermal QST. Long-lasting nerve blocks used for postoperative pain relief, without catheters, are probably the only solution for social security concerns in the short to middle-long term. In the long-term, a better knowledge of the interaction between the different neuro-physiologic systems might lead researchers to long-lasting analgesia.
If no research is performed in the next few years, we might be confronted with the risk of sending patients in pain, home, with the real possibility of an evolution into chronic pain. This would increase the costs of the social security systems in two ways: firstly, due to an increase in health expenses to treat chronic pain; and secondly, due to long-term sick leave because of this chronic, invalidating pain.
Dr Luc Sermeus, MD, PhD
Department of Anesthesia
Antwerp University Hospital
University of Antwerp
+32 3 821 30 42
luc.sermeus@uza.be
http://www.uza.be
This is a commercial article that will appear in Health Europa Quarterly issue 6, which will be published in August, 2018.
























