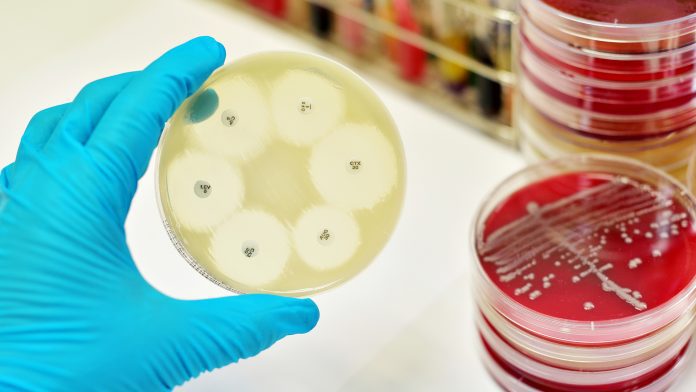
We discuss access and barriers to antimicrobial diagnostics with researchers from the London School of Hygiene & Tropical Medicine
Antimicrobial resistance (AMR) is a natural phenomenon. As microbes multiply, the replication of their genes is not always perfect. These errors in replication are called mutations. Most mutations are harmless, some can kill the microbes while others can confer a survival advantage to the microbe, allowing them to adapt to a new environment, such as growing in the presence of a substance that normally kills them. However, although AMR arises as a natural phenomenon, the main drivers of both its development and spread are ‘man-made’. These include overuse of antimicrobial compounds in humans, animals and plants; lack of access to clean water, sanitation and hygiene; poor infection prevention and control in healthcare facilities and limited availability of vaccines, diagnostics and appropriate treatment.
In 2016, Lord Jim O’Neill published a report stating that if no action is taken, by the year 2050, mortality due to AMR will increase from 700,000 in 2016 to ten million a year. AMR will become the leading cause of death, loss in global productivity will exceed $100 trillion and AMR will push an additional 28 million people into poverty.1 A study of 23 pathogens and 88 pathogen–drug combinations in 204 countries and territories show that an estimated 4.95 million deaths were associated with bacterial AMR in 2019,2 which means that the number of deaths attributable to AMR is increasing at a much faster rate than previously estimated.
Then, with the emergence of the COVID-19 pandemic in 2020, the global AMR crisis suffered another major setback. To say the future of our health is in trouble is an understatement.
What impact has the COVID-19 pandemic had on AMR surveillance and response?
The pandemic led to the over-prescription and overuse of antibiotics.3 The feedback from our interview with experts from Africa, the Middle East, and Latin America pointed out that Azithromycin was prescribed for COVID-19 patients even when there was no evidence supporting its use. A study conducted in 88 countries showed that 72% of hospitalised patients received antibiotics when only 8% were demonstrated to have bacterial or fungal co-infection.4 70% of ICU patients received at least one antibiotic, while only 54% had suspected or proven bacterial infections. Azithromycin was often used with hydroxychloroquine even though neither is recommended.4
In terms of hospital-acquired infections, increased hospital admissions and longer hospital stays increase the risks of healthcare-associated infections, especially since many COVID patients had underlying conditions that put them at risk of acquiring healthcare-associated infections. Hospitals also suffered from outbreaks of multidrug-resistant organisms that were not seen before the COVID-19 pandemic as most hospitals were short of personnel who could maintain AMR stewardship and infection prevention and control programmes. The wide use of biocidal agents for environmental and personal disinfection can select for resistance and enhance cross-resistance to antibiotics, especially in gram-negative bacteria.5

Hospitals suffered from outbreaks of multidrug-resistant organisms that were not seen before the COVID-19 pandemic as most hospitals were short of personnel who could maintain AMR stewardship and infection prevention and control programmes
The pandemic also led to disruptions to health services, such as treatment, for tuberculosis and HIV, which can also lead to selection for drug resistance.6 There were also disruptions to vaccination services, which can increase the risk of infection, potentially leading to an overuse of antimicrobials.5
What are the key issues with traditional diagnostic tests that hinder appropriate antibiotic use in LMICs?
Traditionally, a health provider in a primary healthcare setting in low-and-middle-income countries uses a syndromic approach for patient management where the patient is given broad-spectrum antibiotics presumptively for treating all the major causes of that syndrome. In settings where the health provider has access to a laboratory, a specimen may be collected and sent to the laboratory to confirm the clinical diagnosis. But the traditional diagnostic methods currently available can take hours to days, so antibiotics are still prescribed presumptively while waiting for the laboratory results. The advent of rapid diagnostic tests such as rapid malaria tests and Strep A tests can change this practice, providing more definitive results, but the uptake of rapid tests to guide appropriate antibiotic use in primary healthcare settings has been slow. Reasons for the lack of uptake can include mistrust of the rapid tests most likely due to a lack of understanding of the results – i.e., the rapid test does not fit into the current patient pathway even though it only takes 15 minutes to obtain a result.
In recent years, host biomarkers such as C Reactive Protein (CRP) and Procalcitonin have been studied for their use at the point of care to help clinicians differentiate between bacterial and viral infection and thus reduce unnecessary antibiotic prescriptions.7 This is especially useful for respiratory infections, the majority of which are caused by viruses on which antibiotics have no effect. But again, the uptake is low despite the increasing numbers of acute respiratory illnesses coinciding with COVID-19. One major limitation is that the cost of tests is usually more than the cost of treating a patient empirically and in many countries, antibiotics are readily and cheaply available from drug stores.
Consequently, as more research is ongoing to develop better diagnostic tests that can guide antibiotic treatment, considerations for cost and availability need to be made. Furthermore, policymakers and decision-makers need to reconsider how the value of diagnostics for AMR is assessed and emphasised. Diagnostics need to be valued based on cost prevention and long-term benefits in the healthcare system.
Affordable, point-of-care antimicrobial diagnostics are urgently needed, what are some of the current barriers to their development?
Several obstacles are faced in the antimicrobial diagnostics access pathway, from their development and validation in the laboratory to the point at which they are approved and taken up by those who need them. Traditionally, there has been a lack of early engagement between the industry and key stakeholders during the planning and development phase of new technologies. This is a time for end users and the industry to discuss current health challenges and potential solutions.
Along this access pathway, there are valleys of death that can be encountered that are linked to regulatory approval, policy development, financial, and health system barriers. In many LMICs, regulatory bottlenecks pose significant challenges.8 The regulatory processes are fragmented, ill-defined, and not transparent in many countries.9 This fragmentation and lack of harmonisation across countries have led to significant duplication of studies, resulting in delays in approval and increased cost of getting the product to market. Even when tests are approved, the policies on how the tests are to be used in specific health systems take a long time to be developed. If policy guidance is lacking, procurement and supply chain management also suffer and can further delay the uptake of and access to these rapid tests.
Equally, what challenges do developers currently face?
The International Diagnostics Centre of the London School of Hygiene & Tropical Medicine and Chatham House launched the Accelerating Diagnostics Access Project to understand the challenges developers face. In an organised global consultation with more than 40 diagnostics companies, the critical challenges highlighted were market barriers, access to biological specimens, regulatory hurdles leading to duplication of clinical performance studies, lack of effective communication and advocacy with policymakers, and slow policy development to support antimicrobial diagnostics.
Furthermore, an unpredictable market size can lead to limited or no commitment from antimicrobial diagnostics developers to invest in test development or engage in a production line to manufacture tests.
Finally, innovation to promote the uptake of antimicrobial diagnostic tests in communities needs to be encouraged. Understanding the barriers to knowledge about the use of antimicrobial diagnostics, such as self-tests in the communities, will provide helpful feedback that can enhance their uptake.
Given that the pandemic highlighted the need to expand laboratory capacity and surveillance, what international action is needed to repurpose this capacity towards AMR?
The COVID-19 pandemic has led to an expansion in laboratory technology, capacity, and surveillance in LMICs. International coordination is needed to repurpose these assets in the fight against AMR. In Africa, for example, Africa CDC is working with countries to strengthen clinical and public health laboratory systems and networks across the continent through continued improvements and workforce competency to assure quality and safety. The key activities in this Africa CDC model that will help in the fight against AMR include:
- repurposing the implementation of modern, advanced molecular technologies and multiplex pathogen assays;
- introducing patient-centred approaches for integrated point-of-care testing for syndromic management and surveillance at the community level;
- developing strain banks as repositories for antimicrobial diagnostics and vaccine development of emerging and re-emerging pathogens;
- and supporting lab workforce development.
The progress made during the COVID-19 pandemic that can be leveraged for AMR includes increased coverage and sampling for strengthening surveillance, decentralisation of laboratories, increased sequencing capacity to track variants, biobanking and reference laboratory networks to increase access to samples, sharing of data across multiple sectors, and quality standardised testing.
Notably, the public and private sectors, including regulatory bodies and policymakers, need to be involved in fostering an enabling environment for the rapid translation of local research into products that can be used for AMR and other global health security priorities.
Are there any recent developments within the field of diagnostic research and innovation that you would like to highlight?
The convergence of technologies for digitising test data, Machine Learning and Artificial Intelligence have made it possible to develop a connected diagnostic system to serve as the backbone of a surveillance system that provides early alerts of outbreaks and monitors the effectiveness of disease control strategies and interventions. Countries should utilise this technology convergence to build a strong AMR surveillance system to track resistance trends and assess the impact of AMR strategies and interventions.
The COVID-19 pandemic has led to an expansion in laboratory technology, capacity, and surveillance in LMICs. International coordination is needed to repurpose these assets in the fight against AMR
We should also look to integrate available antimicrobial diagnostics testing through rapid diagnostics multiplex testing. This is an opportunity to test patients presenting with, for example, acute reparatory illness, and be able to distinguish between COVID, flu and RSV to provide appropriate treatment and reduce overuse of antibiotics.
In terms of innovation, the COVID-19 pandemic has shown that community engagement is critical for an effective pandemic response. It is critical that innovative mechanisms engage communities to increase awareness of AMR as a silent pandemic that is killing more and more people every year.
Diagnostics play an important role in the AMR response in reducing inappropriate use of antibiotics and in screening and monitoring resistant healthcare-associated infections in healthcare facilities. These tools can be used to conserve antimicrobial compounds for future generations and save patients from dying from resistant infections. Everyone from researchers to policymakers and patients has a part to play – the future is in all our hands!
References
1. Neill JO’. Antimicrobial Resistance: Tackling a crisis for the health and wealth of nations The Review on Antimicrobial Resistance Chaired. 2014;(December).
2. Murray CJ, Ikuta KS, Sharara F, Swetschinski L, Robles Aguilar G, Gray A, et al. Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. Lancet. 2022;399(10325):629–55.
3. Gerhart J, Delivery SB-NCI in C, 2021 undefined. Overprescription of Antibiotics for Sore Throat Surged During the Covid-19 Pandemic. CatalystNejmOrg [Internet]. Available from: https://catalyst.nejm.org/doi/full/10.1056/CAT.21.0366
4. Rawson TM, Moore LSP, Zhu N, Ranganathan N, Skolimowska K, Gilchrist M, et al. Bacterial and Fungal Coinfection in Individuals with Coronavirus: A Rapid Review to Support COVID-19 Antimicrobial Prescribing. Clin Infect Dis. 2020;71(9):2459–68.
5. Haileyesus Getahun A, Ingrid Smith A, Kavita Trivedi A, Paulina S, Balkhyb & HH. Tackling antimicrobial resistance in the COVID-19 pandemic. Bull World Health Organ. 2020;45–70.
6. The Global Fund. The Impact of Covid-19 on Hiv , Tb and Malaria Services and Systems for Health : a Snapshot From 502 Health Facilities. Glob Fund to Fight AIDS Malaria, Tuberc [Internet]. 2021; Available from: https://reliefweb.int/sites/reliefweb.int/files/resources/covid-19_2020-disruption-impact_report_en.pdf
7. Aulin LBS, de Lange DW, Saleh MAA, van der Graaf PH, **Völler S, van Hasselt JGC. Biomarker-Guided Individualization of Antibiotic Therapy. Clin Pharmacol Ther. 2021;110(2):346–60.
8. Kelly-Cirino CD, Nkengasong J, Kettler H, Tongio I, Gay-Andrieu F, Escadafal C, et al. Importance of diagnostics in epidemic and pandemic preparedness. BMJ Glob Heal. 2019;4:1–8.
9. McNerney R, Peeling RW. Regulatory in Vitro Diagnostics Landscape in Africa: Update on Regional Activities. Clin Infect Dis. 2015;61(Suppl 3):S135–40.
Professor Rosanna Peeling
Professor and Chair of Diagnostics Research
London School of Hygiene & Tropical Medicine
Dr Noah T Fongwen MD MPH
Research Fellow and Lead for Diagnostics Access at Africa CDC
London School of Hygiene & Tropical Medicine
Dr Debi Boeras PhD
Founder & CEO
Global Health & Impact Group
This article is from issue 24 of Health Europa Quarterly. Click here to get your free subscription today.
























