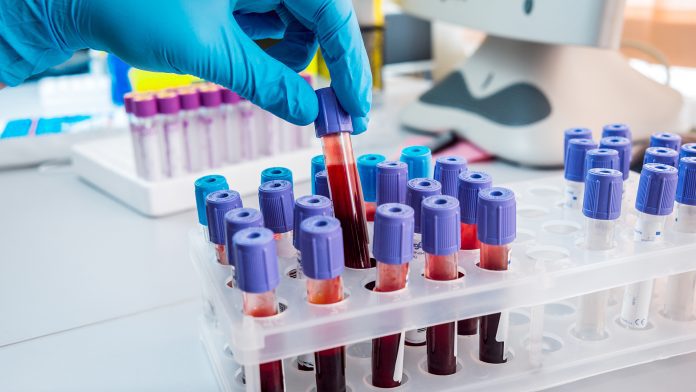
A team of international researchers are calling for revised guides to help improve access to chronic hepatitis B treatment in Africa.
Hepatitis B is a highly endemic virus in Africa, which causes the liver to become infected that is spread through blood, semen, and vaginal fluids. An estimated 82 million people are affected by chronic hepatitis b; however, many people living with the infection are aware of their diagnosis and few have access to treatment. Lack of treatment can lead to more life-altering conditions such as liver cancer.
Now, researchers from across the world, including a team from the University of Liverpool, are calling for increased use of simple, low-cost blood tests which can help to decide which patients with hepatitis B should start treatment. The findings were published in Nature Communications.
Collaborative research from international researchers
The collaborative study called HEPSANET (Hepatitis B in Africa Collaborative Network) involved colleagues from 12 sites in eight African countries. They shared data from different centres that provide care for patients with hepatitis B, the researchers tested how well a combination of cheap and accessible blood tests could predict liver stiffness, a marker of advanced liver disease. Patients with increased liver stiffness are at higher risk of complications such as liver failure and liver cancer, both can be prevented with timely antiviral treatment.
Updating chronic hepatitis B guidelines to improve treatment access
The study revealed that the existing World Health Organization (WHO) guidelines from 2015, which recommend a simple biomarker called APRI to assess liver injury, are not adapted for the African population.
The authors suggested that lower the treatment decision threshold of this biomarker for African patients and improving the hepatitis B guidelines to ensure they are better adapted to Africa. The African continent has been left behind in the fight against chronic hepatitis B despite the continent carrying a high burden of preventable diseases and new infections.
Co-author Dr Alexander Stockdale, a Senior Clinical Lecturer at the University of Liverpool and Malawi-Liverpool-Wellcome Trust Clinical Research Programme, said: “Our findings are timely since WHO guidelines for hepatitis B are currently undergoing revision. A lower APRI threshold is needed and the revised guidelines should take into account our new findings. Patients and clinicians in Africa need simple, accessible guidelines that offer improved access to treatment now.”
Co-author Dr Marc Henrion, a Senior Lecturer in Biostatistics at the Liverpool School of Tropical Medicine and Malawi-Liverpool-Wellcome Trust Clinical Research Programme, added: “Our study really illustrates the power in systematically pooling all available data on a given research topic and analysing them together using robust statistical models. In our case, we have comprehensively shown that existing WHO diagnostic guidelines using the APRI biomarker are inadequate for sub-Saharan African populations. Further, we have estimated and evaluated improved rule-in and rule-out diagnostic thresholds for these populations.”
























