Here, Sekisui Diagnostics, the innovative company behind the OSOM® Trichomonas test, explore the common sexually transmitted infection, trichomoniasis, outlining key symptoms, complications, treatments and prevention options.
Trichomoniasis is a common, curable, non-viral sexually transmitted infection caused by a motile protozoan parasite called Trichomonas vaginalis. Trichomonas (sometimes referred to as “Trich”) infects the vagina and sometimes the urethra during unprotected sex. It is roughly as big as a white blood cell and is thought to be responsible for approximately 15-20% of symptomatic vaginitis infections.
Both men and women can get a Trichomonas infection, but it is more commonly found in women.
Formerly considered a nuisance infection, trichomoniasis is now recognised as a cause of serious health problems. Nevertheless, it continues to be highly underdiagnosed and under-treated.
Incidence: 156 million cases a year
The World Health Organization estimates an incidence of 156 million new cases of T vaginalis each year. In the United States, the Centers for Disease Control and Prevention estimates more than two million trichomoniasis infections in 2018. The incidence of trichomoniasis in Europe is similar to that in the United States. In Africa, the prevalence of trichomoniasis is believed to be much higher.
The prevalence of vaginal T vaginalis infection was estimated to be 11-25% among African study populations.
What are the symptoms of trichomoniasis?
Only about 30% develop any symptoms of trichomoniasis. When symptoms do occur, they range from mild irritation to severe inflammation. Some individuals will develop symptoms within five to 28 days after being infected. Others do not develop symptoms until much later, and those symptoms can come and go. It is important to note that people without symptoms can still pass the infection on to others. Trichomonas symptoms in women can differentiate from other common forms of vaginitis, such as Bacterial vaginosis and Candida. Men with trichomoniasis may notice:
- Itching or irritation inside the penis.
- Burning after urination or ejaculation.
- Discharge from the penis.
Complications of Trichomoniasis
For example, trichomoniasis can cause genital inflammation, which makes it easier to get infected with HIV or to pass HIV on to a sex partner.
Pregnant women with trichomoniasis are more likely to have their babies too early (preterm delivery). Also, babies born to infected mothers are more likely to have a low birth weight (less than 5.5 pounds).
A woman with untreated trichomoniasis has a greater chance of having an infected uterus and Fallopian tubes. This infection, called pelvic inflammatory disease, can cause belly pain, fever, and perhaps the inability to have children (infertility), a pregnancy outside the uterus (ectopic pregnancy), and chronic pelvic pain.
Treatment and Prevention
Since it is an STI, the best way to prevent Trichomonas is to have protected sex. Re-infections with Trichomoniasis are also possible. The best way to avoid re-infections is for the patient to avoid having sex for seven days after treatment has been administered. Trichomoniasis is typically treated with either of the following antibiotics:
Diagnosing trichomoniasis
STD testing, including a trichomoniasis test, may be recommended for people with certain risk factors, including sex without a condom, multiple sex partners, or a history of other sexually transmitted diseases. Because the majority of men are asymptomatic carriers, the diagnosis of T vaginalis is usually not made, and the male partner is identified and treated with metronidazole at the same time as the female partner.
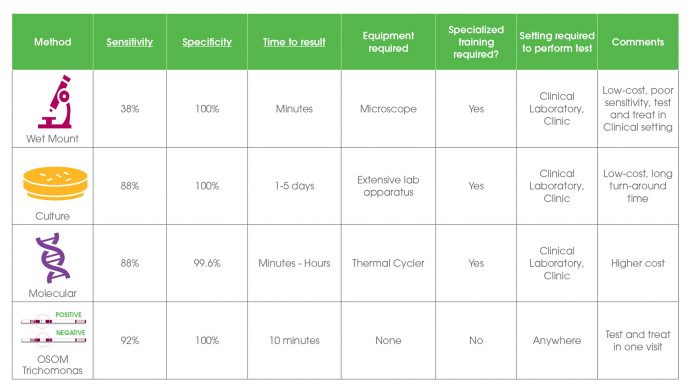
Several testing options are available. Choices are made based on accuracy, timeliness, and cost:
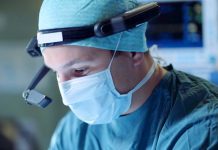
Microscopy
The most commonly used diagnostic test is wet preparation microscopy.
A swab is used to collect material from the vaginal fornix and placed into a small amount of 0.5 to 1.0 ml of normal saline.
A drop of the saline preparation is placed on a slide and viewed with a microscope with a 40× objective.
Culture
This refers to the deliberate growing of cells, especially microorganisms, in a solid or liquid medium (e.g. agar, gelatin), as bacteria in a Petri dish.
Incubation periods ranging from two to seven days are required to identify T vaginalis in culture.
Molecular
Nucleic amplification assay tests (NAATs) are based on rRNA extraction from specimens, followed by transcription-mediated amplification of captured rRNA.
The use of this target provides a natural boost to the limit of detection since 102 to 103 copies exist within each organism.
Lateral Flow
Another treatment includes a immunochromatographic enzyme assay performed on a capillary flow dipstick device with a vaginal swab specimen, such as the OSOM Trichomonas rapid test.
The assay relies on a latex-tagged antibody to bind specifically to trichomonas proteins and a secondary capture antibody to bind the complex to the lateral-flow device.
OSOM® Trichomonas test
The OSOM Trichomonas rapid test has a much-improved sensitivity and excellent specificity and compares favourably to NAATs [nucleic amplification assay tests], with reported sensitivities of 83%–90%. Suitable for Laboratory and Point-of-Care (POC) setting, the test offers the following benefits:
- It has a 95% agreement with culture and wet mount combined.
- A test-and-treat approach in one visit.
- Detects the antigen – does not require a live organism.
- Yields results in 10 minutes or less.
- Offers objective, easy-to-read two-colour results.
There are many advantages of a test and treat approach, including:
- Prevent spread – Quick diagnosis allows the clinician to provide appropriate and immediate treatment to prevent further spread of Trichomoniasis.
- Patient compliance – Ensures the patient starts medication immediately.
- Convenience – Patients can self-swab for sample collection (CE marked product only).
- Prevent inappropriate treatment – Accurate diagnosis results in avoidance of syndromic management.
Check out our webinar about the challenges of diagnosing Vaginitis.